What is Adderall? (Amphetamine/Dextroamphetamine)
Adderall (amphetamine/dextroamphetamine) is a basic amphetamine with powerful stimulant effects. It’s one of the most effective treatments currently available for treating attention deficit hyperactivity disorder (ADHD). Here’s everything you need to know.
Amphetamine/dextroamphetamine salt combo (or its brand name Adderall) is the first line of defense for most people with ADHD. Despite this, much of the way it works and how it helps are largely underresearched.
Adderall comes in two options — extended-release (XR) and immediate-release (IR) — but both have the same formulation and mechanisms of action.
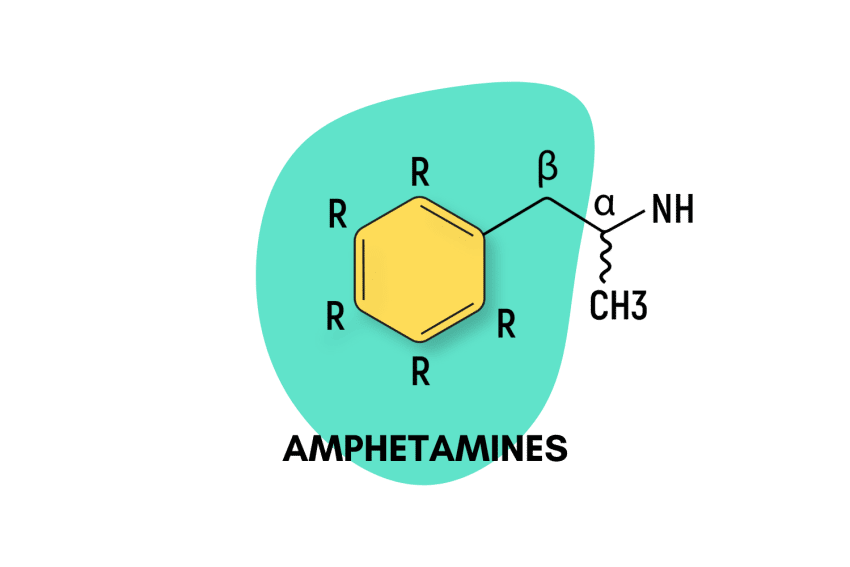
Adderall is just one of many members of the greater amphetamine family of drugs — which includes such members as lisdexphetamine (Vyvanse), bath salts (synthetic cathinones), DOX psychedelics, MDMA (ecstasy), and many others.
In this article, we’ll break down this common drug with information on the following:
- What Is Adderall — Including the difference between the two salts, the purpose of their combination, and possible theories for the efficacy of its formulation.
- How does Adderall work — Including why its main mechanisms of action (increasing dopamine and epinephrine levels) help with ADHD
- Is Adderall safe — With cardiovascular side effects, risk of abuse, psychological concerns, potential neurological stresses, and physiological problems treatment may entail.
- Indications for Adderall — Both official (namely, ADHD and narcolepsy) and unofficial reasons psychiatrists prescribe Adderall.
- Adderall Tolerance Avoidance & Reset
- How Adderall Compares To Other Stimulants — Including Ritalin, Concerta, Focalin, and Vyvanse.
- When to Avoid Adderall
- Medications to Avoid When Taking Adderall
- When to Consider Getting a Prescription for Adderall
While we hope to provide you with all the information you’re looking for, stimulant medications are not for everyone. Always discuss the potential of starting treatment with a healthcare professional before doing so — they may tell you it’ll do more harm than good.
What is Amphetamine/Dextroamphetamine Combo (Adderall)?
Amphetamine is an enantiomer — meaning it has two molecular arrangements of the same formula, forming a mirror image of each other. There is the l-amphetamine (levoamphetamine) enantiomer and the d-amphetamine (dextroamphetamine) enantiomer.
Adderall is a 1:1 mixture of racemic (equal parts) amphetamine with just d-amphetamines — forming a total ratio of 3:1 d- to l-amphetamines.
So, if you were taking a 15 mg dose, you would be taking 7.5 mg of d-amphetamine and 7.5 mg of equal parts l-amphetamine and d-amphetamine.
What’s the Difference Between L-Amphetamine, Amphetamine Combo, & D-Amphetamine?
D-amphetamine is stronger than l-amphetamine, and “amphetamine” on its own usually means the mixture of the two. By some reports, d-amphetamine may be as much as 3–5x as strong as its “left-handed” enantiomer [1].
When dealing with something as intricate as a molecule, the arrangement matters — don’t discount l-amphetamine, though. One study found it to be twice as effective as d-amphetamine for the release of norepinephrine (a major component of amphetamine action) from the basal frontal cortex of the brain [2].
Importantly, this is one section of the brain and one function of amphetamine, but it’s important nonetheless. Mixed amphetamines like Adderall use both enantiomers to achieve a longer-lasting — potentially slightly varied — effect.
Why Combine L-Amphetamine & D-Amphetamine?
Research is conclusive when it comes to the benefits of combination amphetamines over taking d-amphetamine alone. What we have yet to prove is why this happens — if d-amphetamine is stronger, why wouldn’t we just include it?
While we don’t have an answer to this question, there are a few prominent theories:
L-Amphetamine Helps Through Competition
While l-amphetamine doesn’t have the same efficacy as d-amphetamine, this may ultimately work in its favor. Nearly immediately after d-amphetamines attach to the dopamine receptors, they begin regulating dopamine activity — l-amphetamines may take over some of the receptors and help slow this effect [3].
This could even be an isolated location “that allows for more rapid downregulation” — or reducing the number — of dopamine receptors. By slowing this effect, the isomer could help its other half be more effective and stick around longer.
Or, this could simply be a matter of “taking up space” and preventing d-amphetamine from accessing all the receptors. As we’ll get into below, d-amphetamine also slows the enzyme responsible for breaking it down before it gets to the receptor.
If the more potent option has to wait around for a receptor to open — and can survive — it could contribute to the added duration [1].
L-Amphetamine Alters Dopaminergic Response
We consider l-amphetamine to be the weaker option of the two, but we’re only checking for specific indicators. We may yet uncover alternative effects we haven’t been looking for previously.
One study discovered a 1:1 preparation of the two wasn’t more effective than either, but the 3:1 formulation of Adderall was, proposing it “may be altering [dopamine transporter] function [4].”
Researchers in this study noted that more l-amphetamine could be detrimental to the overall effect on attention. One explanation for why it may do so is the pharmacological effect of l-amphetamine becoming detrimental after a certain dosage.
While it seems like more competition on the receptor would be a good thing, it might not be if other properties of the enantiomer are active. Alternatively, there may simply be a point where l-amphetamine takes over too many receptors, and d-amphetamine can no longer wait out its turn.
Other Reasons l-Amphetamine Helps d-Amphetamine
The final option is the one we hate the most: we simply don’t know. Exploratory research with low potential for financial gain is hard to get funding for, even for popular medications like this one.
Additionally, we still don’t have a firm grasp on several components of neurology or a solid way to study these effects in living humans. Most research on the topic revolves around rodent studies, and, as you might expect, they’re not very good at explaining how they feel.
L-amphetamine may act on our neurological system in ways we have yet to uncover, or it may serve an important function we’ve never considered.
How Does Adderall Work?
Amphetamines are a large and diverse group of psychostimulants. The main way these drugs work is by increasing the activity of dopamine and norepinephrine in the system [5].
There are a few ways amphetamines can boost dopamine and norepinephrine activities:
- By increasing the production and release of dopamine, norepinephrine, and other neurotransmitters.
- By inhibiting monoamine oxidase transporter 2, which is responsible for storing and transporting excess storage into the brain.
- By preventing the production of proteins responsible for the reuptake (or absorption) of these neurotransmitters — thus increasing the time they remain active in the system.
- By reversing the direction of cellular pumps that move dopamine and norepinephrine around the synapses.
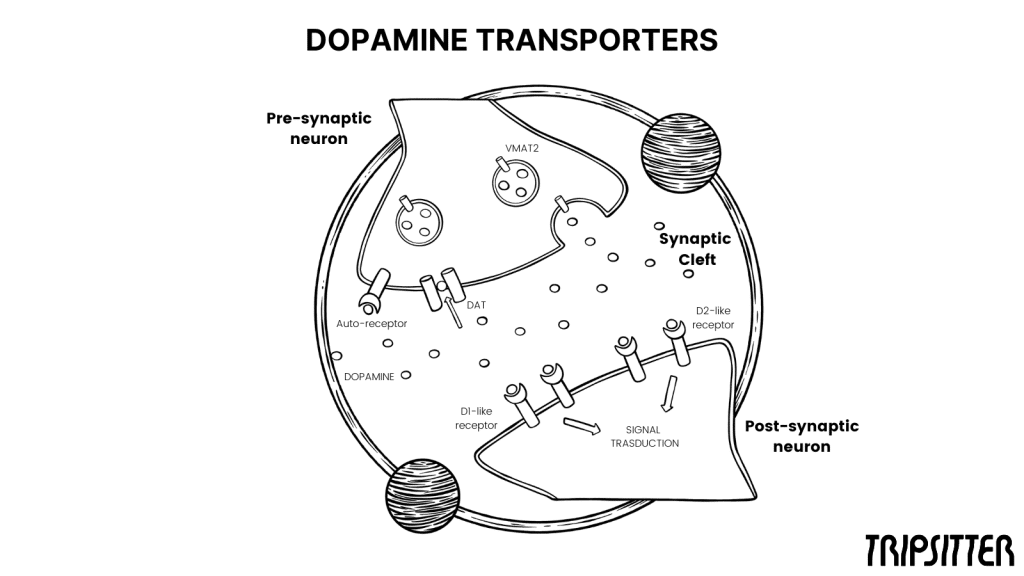
What Do Dopamine and Norepinephrine Have to Do With ADHD?
ADHD is a complex disorder with several underlying causes and symptoms, including far more than dopaminergic and adrenergic ones. However, research shows abnormalities with these two systems are common among people with ADHD [6], and — even if there are problems outside of this — stimulants are the top treatment for it.
Dopamine is responsible for, among many other things, regulating and rewarding the mind. When you develop a habit or pattern, dopamine is partially responsible for it, giving a tiny reward of dopamine when you do the action and conditioning your brain to enjoy and seek it out [7].
Norepinephrine is responsible for regulating the focus of attention — either in small amounts (like when you’re sitting through a lecture) or large amounts (like in a life-or-death situation [8].) This important neurotransmitter also operates as a hormone, meaning it moves both through the bloodstream and across neurons.
They don’t answer the entire problem or address every symptom — after all, family and societal environment play a major role [9], and no pill can solve that. Additionally, we are still unaware of the full mechanism of action with amphetamines.
Even the dopaminergic and adrenergic functions we have proven usually include theoretical mechanisms for how they occur. It’s also possible amphetamines also answer other systems or functions responsible for symptoms of ADHD we haven’t recognized yet.
While there’s a lot we have yet to discover about the role of these neurotransmitters in treating or causing ADHD, addressing them appears to be wildly successful for treatment.
Is Adderall Safe?
Synthetic amphetamines are nothing new, and — despite a lot of fearmongering — they’re largely safe and effective. Still, there are risks associated with Adderall, and it’s important to know about them and how to avoid them before starting treatment.
Cardiovascular Side Effects of Adderall
Amphetamines elevate heart rate and blood pressure, causing stress on the heart. Research is still mixed on the topic — a recent review found 1/6 of studies in children and 2/3 for adults linked the two [10] — but elevating heart rate has the inherent risk of cardiovascular problems.
We don’t know the effect of this over time, but daily amphetamine use and repeated stress on cardiovascular functions could be harmful. As a result, it’s important to ensure you’re treating your heart right when taking Adderall and not adding to the stress it’s under when you’re medicated.
If you have any cardiovascular concerns or conditions, talk with your doctor before starting Adderall and consider alternative options.

Risk of Abuse
There’s an enjoyable effect to Adderall and heavy regulations on prescriptions, so it’s no surprise some use Adderall recreationally. Problematic use of Adderall can have unsafe or potentially even deadly consequences for users.
No, we’re not talking about the time you took Adderall so you can stay up and study for an exam. While not a healthy way to retain information, this shouldn’t be considered “abuse” when it’s the main reason people receive a prescription — that’s just “use.”
Abuse involves dealing with exceptionally high doses, long-term repeated use without any breaks, or putting health or community in danger to continue seeking it out. Often, this involves exploring alternative routes of administration like insufflation (snorting) or others, but this alone shouldn’t constitute abuse, even if it’s less safe.
One of the biggest risks of Adderall abuse involves combining it with alcohol.
When on amphetamines, the effects of alcohol don’t come on right away, often leading people to drink more. When the drug wears off, drunkenness comes on suddenly and may put a person at higher risk of alcohol poisoning or passing out in dangerous situations.
Additionally, the dopamine release from Adderall can reinforce the action, eventually leading to continued problematic use and dependency.
Psychological Side Effects of Adderall
While Adderall may help with ADHD, there are several implications of flooding your brain with dopamine and norepinephrine. These neurotransmitters may cause a spike in anxiety, paranoia, and mood swings.
This becomes especially dangerous when combined with Adderall’s tendency to quell appetite. It’s not hard to not eat all day, simply not thinking of it, and have no idea why moods are swinging so wildly.
Explore options and set a routine to make sure you’re taking in food throughout the day to help avoid this. While these effects are still possible for people with food in their bellies, they’re far less intense or common.
Adderall & Oxidative Stress/Neurological Inflammation
Several amphetamines have shown toxic and inflammatory neurological effects, including Adderall, in some non-human studies. Theoretically, the effects of Adderall may put stress on some of our brain functions, reducing their capability, capacity, or efficacy and potentially leading to long-term effects.
This is far from fact, and some preliminary research on animals contends d-amphetamines have different mechanisms for preventing this. However, with it being a clear concern for both 3,4-methylenedioxymethamphetamine (MDMA) and methamphetamine, it may be a problem across the board with this class of drugs [11].
Oxidative stress and neurological inflammation are the two biggest potential concerns with amphetamines and neurotoxicity. These refer to being unable to remove a large number of unstable molecules and swelling of nerve tissue, respectively.
If this is a real problem for Adderall, these are major concerns with ties to serious mental degenerative diseases. However, it’s important to note we still don’t know this for sure, and the effects of Adderall are far more subtle than those of meth or MDMA, so its negative effects likely follow suit.
Adderall & Physical Side Effects
Weight loss is one of the most common side effects of Adderall use, along with nausea, dizziness, sweating, upset stomach, and other physical concerns. Everyone reacts differently, and some don’t experience any problems, but it’s important to start with a low dose to familiarize yourself with it first.
After, you can work your way up slowly to the right dosage for the effects you need with less of the ones you don’t.
What Is Adderall For?
Adderall has two indications prescribers suggest it for and some others which aren’t technically approved but for which it may still help. Its two indications are ADHD/ADD and narcolepsy, but physicians may also use it for other mental health concerns.
ADHD/ADD & Adderall
This is the biggest indication for Adderall prescriptions and the largest potential for the drug. To indicate a need for a prescription, patients must have difficulty with attention and hyperactivity, typically present before age 7.
Especially for younger children, ADHD may manifest as aggressive behavior, anger, or an inability to restrain yourself. Adderall’s release of dopamine for behavior and norepinephrine for focus makes it a fantastic treatment option.
While many claim it has an advantage over the other treatments for this condition, this is currently unsubstantiated by research.
Narcolepsy and Adderall
Narcolepsy — or falling asleep uncontrollably — is another concern Adderall often helps address. The alert and focused nature of amphetamines make them helpful for ensuring you stay awake during key moments like when you’re working, driving, or otherwise in a dangerous situation.
Physicians may prescribe an extended-release option to ensure people are awake all day and/or an instant-release to use whenever you need 3–5 hours.
Off-Label Adderall Use
While Adderall doesn’t answer them directly, it may help treat the symptoms of other mental health conditions. Depression, anxiety, and other disorders may benefit from the mechanisms of action Adderall uses to treat its main indications, even if it’s not a proven treatment for them.
It’s important to ensure you don’t use Adderall in this way on your own and talk at length about it with your provider. While they may recommend it on their own, it also has the potential to worsen many conditions, and you should not take it lightly.
Often, other symptoms — like anxiety — manifest as a condition of ADHD, but stimulants can make them worse.
Adderall Tolerance Reset & Prevention
Prescription amphetamines of all types omit a recommendation for a tolerance break in their guidelines, but most people will tell you these are essential. Over time, your brain and body become dependent on the amphetamines you’re providing, adjusting to them and requiring larger doses or making them ineffective.
This happens on rapid and long bases — forming an initial tolerance that wears off over time but gradually grows. In some cases, people even form a complete tolerance, meaning they can’t achieve an effect with their medication regardless of dosage.
The best way to prevent tolerance build-up is to take frequent breaks of 1–2 days (ideally weekly) and longer ones whenever possible. However, this isn’t always possible for some who are using the drug for life-saving treatment.
If you find yourself building a tolerance to your medication, you can reset your tolerance by taking a break of 2–4 weeks or talking with your provider about switching medications. Some options — like methylphenidate, may still work as you reset your tolerance to Adderall [12].
Adderall Vs. Other Stimulant Medications
While stimulant medications share broad similarities, they have some differentiating factors which can determine who it’s best for. Among the various formulations, the main two options are forms of methylphenidate and d-amphetamines.
While the two work in similar ways, methylphenidate primarily works by inhibiting reuptake though it still releases neurotransmitters in a similar — albeit less overwhelming — way [5]. Like amphetamine, methylphenidate also has a d- and l- enantiomer, with d-methylphenidate being stronger.
Let’s take a look at some different brand names of ADHD medication and how they differ from Adderall.
Adderall vs. Ritalin
Ritalin is comparable to immediate release options for Adderall, though it seems to act more immediately and reach a peak effect quicker. As a result, this may be a better option for people who need an as-needed option for ADHD symptoms, as they won’t have to wait as long for the onset.
With this comes a more rapid return to baseline, however, so Adderall typically lasts longer. Still, some note the different mechanisms of action result in Ritalin having less of a “crash” than Adderall — though research has yet to confirm this.
Adderall vs. Concerta
This is the XR methylphenidate option, acting similarly to Adderall’s extended-release options. Concerta and Adderall XR may both last up to 12 hours. However, Concerta’s range is 10–12 as opposed to 8–12 with Adderall.
This may point to a more reliably long-lasting effect from Concerta, but ultimately, the difference is up to the individual and which drug works best for them. Everyone has their preference, and it’s unlikely there is a major difference between the two.
Adderall vs. Focalin
Focalin contains only the stronger of the two enantiomers of methylphenidate (the d- enantiomer). Some claim it has fewer side effects than other options and is milder, but there isn’t any research confirming this.
Similar to the other methylphenidate options, the difference in this likely comes down to preference. It’s also possible the perception of a cleaner effect comes from a lower potency through the removal of l-methylphenidate — we currently don’t have a way to know.
Adderall Vs. Vyvanse
Vyvanse contains lisdexamfetamine, a pro-drug for d-amphetamine — meaning it converts after metabolization. Unlike Adderall IR, which begins entering your system immediately, or XR, which uses a slow-release mechanism, Vyvanse must first pass through the liver to be effective.
As a result, this medication may have a more standardized effect for people by bypassing our unique metabolic makeups before splitting into its active component.
Another benefit of Vyvanse is its long-acting nature though many compare it to Adderall XR as a relatively similar option. Unlike Adderall, Vyvanse doesn’t include the l- enantiomer of Amphetamine.
What are the Contraindications of Adderall?
Avoid Adderall if you have any heart conditions, including:
- Cardiovascular disease
- Hypertension
- Arteriosclerosis
Additionally, you shouldn’t take Adderall if you:
- Are sensitive to amphetamine or other stimulants
- Have received a glaucoma diagnosis
- Have a history of drug abuse, paranoia, or agitated behavior
These conditions could result in deadly after-effects from Adderall, and it’s important to discuss the possibility with your healthcare provider before taking Adderall.
Medications to Avoid When Taking Adderall
The biggest medication to avoid using with Adderall are other monoamine oxidase inhibitors (MAOI) — particularly ones with long-lasting effects. These are often found in the form of antidepressants, and they can slow the metabolization of amphetamines, drastically increasing their potency.
A stronger effect is not always a good thing — with amphetamines, users may find themselves clenching their teeth, sweating, or experiencing heavy anxiety. It’s important to avoid anything that may alter the efficacy of any drug you’re taking.
Aside from breaking down drugs, the MAO enzyme also helps regulate blood pressure and other critical functions. As a result, inhibiting it while simultaneously taking a drug with those effects can be deadly.
Other medications to avoid include:
Medications Affecting PH Balance
Several medications work through alterations in the balance within your gut. The result of this can ease several symptoms but also may increase or decrease the effectiveness of your medication.
When on Adderall, medications that acidify or alkalinize your urinary or gastrointestinal tract. The most common of these is sodium bicarbonate — brand names like Tums, Pepto Bismal, etc. — which reduce the acidity of your stomach and, therefore, the amount of amphetamine it breaks down.
On the other side of this are alkalizing agents, which elevate the acidity, drastically reducing Adderall’s effectiveness.
Antidepressants
Other antidepressants may also affect the potency of amphetamines through actions other than inhibiting the MAO enzyme. Trycliclic depressant medication may elevate the potency of amphetamines, and the reverse could be true as well.
Both Adderall and antidepressants often alter dopamine levels and function, and taking them together may cause several issues. Since antidepressants come in a variety of forms, make sure to discuss them with your doctor before pairing the two.
Other Medical Interactions with Adderall
Over 100 medications currently have links to contraindications with Adderall. Since Adderall works on so many essential functions, it has a high likelihood of interaction.
Some of these amount to very little and are ultimately safe; others can be quite serious. Discuss any medication (even over-the-counter) with your provider before taking it.
Antacids, nasal decongestants, and other common medications all have the potential to boost negative effects.
TLDR: What is Adderall (Amphetamine)
This is a decision between you and your healthcare provider, but Adderall is an effective treatment for ADHD with very low risk. However, you should always avoid buying Adderall outside of the medical market as illicit samples very rarely contain d-amphetamine.
If you’re on a medication you already find effective, it’s unlikely you’ll find much benefit in switching over to Adderall. However, for most, Adderall is an excellent option for the first treatment of ADHD symptoms.
If you do get a prescription, take plenty of tolerance breaks, ensuring your dosage needs adjustment as little as possible. Talk with your healthcare professional today and see what they have to say — you may find your symptoms only require lifestyle changes or therapy.
References
- Heal, D. J., Smith, S. L., Gosden, J., & Nutt, D. J. (2013). Amphetamine, past and present – a pharmacological and clinical perspective. Journal of Psychopharmacology, 27(6), 479–496. https://doi.org/10.1177/0269881113482532
- Easton, N., Steward, C., Marshall, F., Fone, K., & Marsden, C. (2007). Effects of amphetamine isomers, methylphenidate, and atomoxetine on synaptosomal and synaptic vesicle accumulation and release of dopamine and noradrenaline in vitro in the rat brain. Neuropharmacology, 52(2), 405–414. https://doi.org/10.1016/j.neuropharm.2006.07.035
- Glaser, P. E. A., Thomas, T. C., Joyce, B. M., Castellanos, F. X., & Gerhardt, G. A. (2005). Differential effects of amphetamine isomers on dopamine release in the rat striatum and nucleus accumbens core. Psychopharmacology, 178(2–3), 250–258. https://doi.org/10.1007/s00213-004-2012-6
- Joyce, B. M., Glaser, P. E. A., & Gerhardt, G. A. (2007). Adderall produces increased striatal dopamine release and a prolonged time course compared to amphetamine isomers. Psychopharmacology, 191(3), 669–677. https://doi.org/10.1007/s00213-006-0550-9
- Faraone, S. V. (2018). The Pharmacology of Amphetamine and Methylphenidate: Relevance to the Neurobiology of Attention-Deficit/Hyperactivity Disorder and Other Psychiatric Comorbidities. Neuroscience and Biobehavioral Reviews, 87, 255–270. https://doi.org/10.1016/j.neubiorev.2018.02.001
- Cortese, S. (2012). The neurobiology and genetics of Attention-Deficit/Hyperactivity Disorder (ADHD): What every clinician should know. European Journal of Paediatric Neurology: EJPN: Official Journal of the European Paediatric Neurology Society, 16(5), 422–433. https://doi.org/10.1016/j.ejpn.2012.01.009
- Juárez Olguín, H., Calderón Guzmán, D., Hernández García, E., & Barragán Mejía, G. (2016). The Role of Dopamine and Its Dysfunction as a Consequence of Oxidative Stress. Oxidative Medicine and Cellular Longevity, 2016, 9730467. https://doi.org/10.1155/2016/9730467
- Hussain, L. S., Reddy, V., & Maani, C. V. (2023). Physiology, Noradrenergic Synapse. In StatPearls. StatPearls Publishing. http://www.ncbi.nlm.nih.gov/books/NBK540977/
- Huang, Y., Xu, H., Au, W., Xu, C., & Wu, K. (2018). Involvement of family environmental, behavioral, and social functional factors in children with attention-deficit/hyperactivity disorder. Psychology Research and Behavior Management, 11, 447–457. https://doi.org/10.2147/PRBM.S178080
- Westover, A. N., & Halm, E. A. (2012). Do prescription stimulants increase the risk of adverse cardiovascular events?: A systematic review. BMC Cardiovascular Disorders, 12, 41. https://doi.org/10.1186/1471-2261-12-41
- Moratalla, R., Khairnar, A., Simola, N., Granado, N., García-Montes, J. R., Porceddu, P. F., Tizabi, Y., Costa, G., & Morelli, M. (2017). Amphetamine-related drugs neurotoxicity in humans and in experimental animals: Main mechanisms. Progress in Neurobiology, 155, 149–170. https://doi.org/10.1016/j.pneurobio.2015.09.011
- Handelman, K., & Sumiya, F. (2022). Tolerance to Stimulant Medication for Attention Deficit Hyperactivity Disorder: Literature Review and Case Report. Brain Sciences, 12(8), 959. https://doi.org/10.3390/brainsci12080959