Nitrazepam (Mogadon) Fact Sheet & Harm Reduction Guide
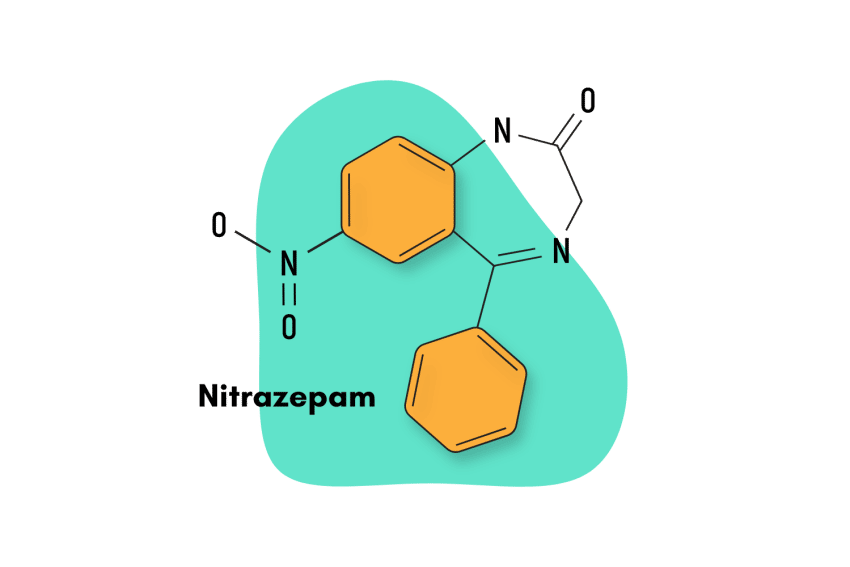
Nitrazepam — sold under the trade name Mogadon — is a 1,4-benzodiazepine derivative that contains a nitro group in its chemical structure and elicits the full range of traditional benzodiazepine-related effects.
This benzodiazepine is classified as an intermediate-acting compound, possessing an estimated elimination half-life of around 24-40 hours.
Nitrazepam has not received FDA approval in the United States, but it is used in several countries. Its primary uses are the short-term management of insomnia, the treatment of epileptic spasms in infants (West’s syndrome), and the short-term relief of severe anxiety.
Nitrazepam Specs
| Status | Approved medication but not in the United States |
| Common Dosage | 5-15 mg |
| PubChem ID | 4506 |
| CAS# | 146-22-5 |
IUPAC Name
7-nitro-5-phenyl-1,3-dihydro-1,4-benzodiazepin-2-one
Other Names
Alodorm, Apodorm, Arem, Cerson, Insoma, Insomin, Mogadon, Nitrados, Nitrazadon, Nitrosun, Nitravet, Ormodon, Paxadorm, Remnos, Epam, Somnite
Metabolism
Nitrazepam is hepatically metabolized by oxidative pathways and excreted mainly as conjugated and non-conjugated 7-aminonitrazepam and 7-acetamidonitrazepam. Polymorphic acetylation is not likely to be of clinical importance. Enzyme induction or significant loss of efficacy has not been found with long-term use.
Duration of Effects
The elimination half-life of nitrazepam is roughly 24-40 hours, considered intermediate-acting. Accumulation as a result of daily nitrazepam use does occur [1].
Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Nitrazepam Work?
Nitrazepam’s primary mechanism of action is the traditional GABA-mediated pathways used by the vast majority of benzodiazepines [2]. However, research suggests that nitrazepam also exerts some pharmacological characteristics through secondary pathways.
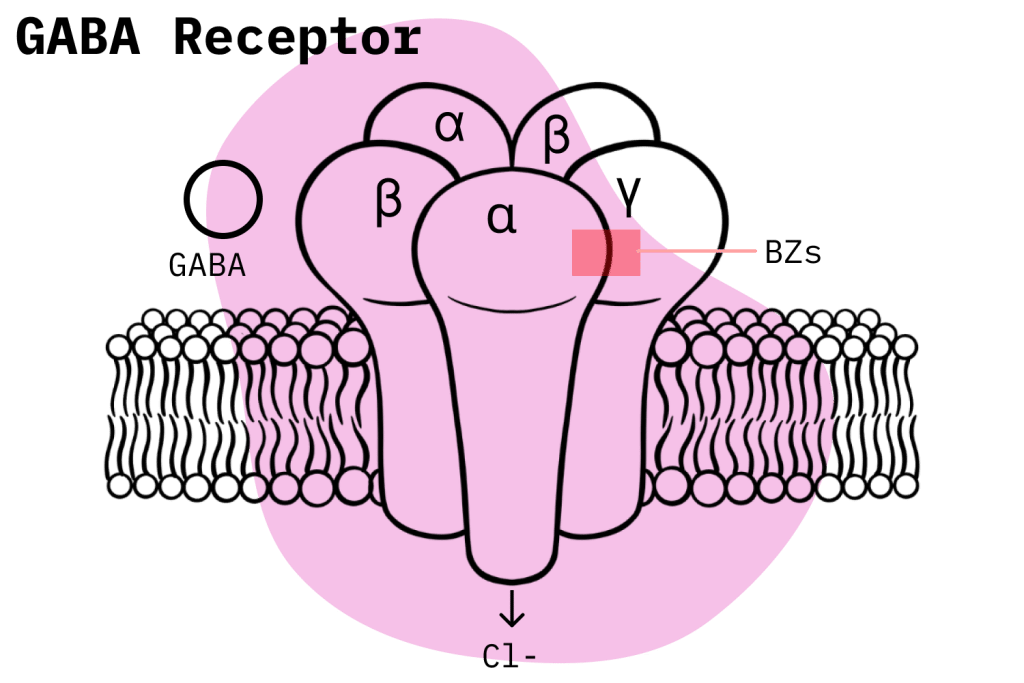
To understand how benzodiazepines work, it’s essential to be familiar with their primary mechanism of action. In simplified terms, when benzodiazepine molecules enter the body, they bind to the benzodiazepine site on GABA neurotransmitters located in the brain and central nervous system (CNS).
GABA is the chief inhibitory neurotransmitter used by the body to “slow down” activity in the brain and CNS. Once benzodiazepine molecules bind with GABA, they produce an allosteric effect that potentiates the natural inhibitory function of GABA receptors. We should note that different molecules interact with GABA receptors in different ways. The allosteric effect produced by benzodiazepines is not the same mechanism used by, for example, barbiturates when they interact with GABA.
GABA receptors, under the influence of benzodiazepines, depress the brain and CNS by increasing the opening frequency of their chloride channels. This permits the passage of negatively charged chloride ions into the inside of the cell, which leads to hyperpolarization. The practical effect of hyperpolarization is that neurons are less likely to fire off action potentials, the electrical signals they use to communicate. This, in turn, leads to a generalized depressive action, along with anxiolytic, sedative, amnesic, anticonvulsant, and muscle-relaxant effects.
Nitrazepam Specifics
Although most benzodiazepines share this common pathway, research has begun to suggest that their individual differences in terms of pharmacokinetics, their affinity for different GABA-A subunits, and the secondary pathways they utilize are quite significant when it comes to their ultimate effects profile and the clinical situations in which they will ultimately be effective [3].
With this in mind, it becomes important to parse out what we know in terms of the specific qualities of nitrazepam.
First off, nitrazepam is a full benzodiazepine agonist rather than a partial one [4], which means that when it binds and activates a receptor, it does this to the maximum response that the receptor is capable of achieving. In general, full benzodiazepine agonists are more potent than partial agonists.
Research has also shown that an opioid-like mechanism of action may also play a significant pharmacological role in nitrazepam’s effects [5]. Additionally, nitrazepam is now known to cause a decrease in the level of glycine and aspartic acid, two amino acids found in the brain.
Furthermore, high doses of nitrazepam can cause a decrease in histamine turnover as a result of nitrazepam’s actions at GABA-A receptor sites [6]. Nitrazepam also has been found to have antipruritic properties, which are believed to come via its central mechanism of action [7]. Lastly, studies have shown that nitrazepam can suppress cortisol formation [8].

Is Nitrazepam Safe? Risks & Side Effects
Nitrazepam is not currently listed under the Controlled Substances Act in the United States but is classified in comparable drug legislation in other countries. In Canada, nitrazepam is classified as a Schedule IV compound, which means that despite having legitimate medical uses, it still has the potential for misuse, physical dependence, and withdrawal symptoms.
Although they have meaningful differences, benzodiazepines all share a baseline risk level that must always be considered as it is quite significant. When benzodiazepines are properly taken (in strict accordance with a prescription), they are relatively safe because they don’t often cause severe adverse effects or health-related events. However, the reality is that benzodiazepine misuse is a very real possibility, which can make them quite dangerous.
In recent years, an explosion in polydrug abuse in the United States has proven, without a doubt, just how dangerous these compounds can be.
A 2020 study by the CDC concluded that benzodiazepines played a part in 12,290 drug overdose deaths in that year. Another study by the National Institute on Drug Abuse can help contextualize this problem in the larger opioid crisis. It found that benzodiazepines were involved in 16% of overdose deaths, the vast majority primarily caused by opioids.
Indeed, opioids are generally more dangerous than benzodiazepines, but what must be understood is that what is truly lethal is the combined effect that arises when two CNS-depressant compounds, such as opioids and benzodiazepines, are combined. Concomitant use of compounds that depress the CNS puts the user at serious risk of respiratory depression, the number one cause of death among drug overdoses.
Side Effects of Nitrazepam
Canadian health authorities have identified several common side effects of nitrazepam:
- Ataxia
- Changes in libido
- Constipation
- Depression
- Diarrhea
- Dizziness
- Drowsiness
- Falling (especially in elderly patients)
- Fatigue
- Headache
- Heartburn
- Lethargy
- Lightheadedness
- Mental confusion
- Nausea
- Nervousness
- Staggering
- Upset stomach

These effects occur predominantly at the start of treatment and tend to fade as it goes on. Furthermore, sedative effects can be decreased by a dosage reduction, and it has been found that children and the elderly are more likely to experience adverse effects.
Rarer instances of the following side effects have also been reported:
- Agitation
- Aggressiveness
- Disorientation
- Excitement
- Granulocytopenia
- Hallucinations
- Hangover effect
- Hyperactivity
- Hypotension
- Increased muscle spasticity
- Irritability
- Leucopenia
- Psychoses
- Rages
- Severe sedation
- Violent behavior
Benzodiazepine Withdrawal & Dependence
Patients undergoing a benzodiazepine treatment would do well to exercise extreme caution against the possibility of developing a benzodiazepine dependence. Many believe that avoiding misuse is enough, but, in reality, that’s hardly the case. Even when patients engage in no misuse, there is still a considerable chance of developing physical dependence. Take this study, for instance. It examined the likelihood of developing dependence in patients who took benzodiazepines for longer than four weeks and found that one-third of participants developed dependence and consequent withdrawal symptoms after completing treatment [9].
In this sense, health authorities recommend that consecutive nitrazepam usage be limited to seven to 10 days as a preventative measure to avoid physical dependence, tolerance, and the accumulation of nitrazepam within the body.

Harm Reduction: Nitrazepam
This section will review some basic but practical and easy-to-implement harm reduction recommendations that will help users minimize their risk levels.
Firstly, the obvious recommendation for any prescription benzodiazepine user is to try their hardest to avoid all possible instances of misuse. And this doesn’t refer exclusively to recreational misuse. Slight alterations of prescription instructions, such as taking your medication at the wrong time or in the wrong formulation, can still be considered misuse. Essentially, prescription users should always follow the instructions given with their benzodiazepines.
Before starting treatment, prescription users should also speak to their doctor and ask them to limit the dosage and the duration of treatment as much as possible without significantly harming the treatment’s probability of success. The longer a drug is consumed and the higher the doses, the likelier a dependence, physical or mental, will form. Limiting these two factors is the best way to hedge against this possibility.
Even though we don’t condone the recreational use of benzodiazepines, we still want recreational users to have harm-reduction knowledge, which can help them reduce the danger they put themselves in.
A good idea for recreational users is to procure flumazenil and learn how to use it. Flumazenil is a benzodiazepine receptor antagonist, which means that it has the potential to revert the effects of a benzodiazepine overdose. However, compounds like flumazenil can be hard to find. The best possibility is to contact harm reduction clinics and organizations.
Recreational users should also try their hardest not to mix potent pharmacological compounds, as this will always increase the danger they’re putting themselves in. And as we learned before, concomitant use of CNS-depressant compounds like opioids, alcohol, barbiturates, and benzodiazepines is especially deadly. These types of compounds shouldn’t be mixed, even if one of them is not necessarily pharmacological. For instance, the kratom plant, a natural herbal compound with CNS-depressant properties, can still be deadly when mixed with any of the drug types just mentioned.
Benzodiazepine Harm Reduction Tips
- 🥣 Don’t mix — Mixing benzodiazepines with other depressants (alcohol, GHB, phenibut, barbiturates, opiates) can be fatal.
- ⏳ Take frequent breaks or plan for a short treatment span — Benzodiazepines can form dependence quickly, so it’s important to stop using the drug periodically.
- 🥄 Always stick to the proper dose — The dosage of benzos can vary substantially. Some drugs require 20 or 30 mg; others can be fatal in doses as low as 3 mg.
- 💊 Be aware of contraindications — Benzodiazepines are significantly more dangerous in older people or those with certain medical conditions.
- 🧪 Test your drugs — If ordering benzos from unregistered vendors (online or street vendors), order a benzo test kit to ensure your pills contain what you think they do.
- 💉 Never snort or inject benzos — Not only does this provide no advantage, but it’s also extremely dangerous. Benzos should be taken orally.
- 🌧 Recognize the signs of addiction — Early warning signs are feeling like you’re not “yourself” without the drug or hiding your habits from loved ones.
- ⚖️ Understand the laws where you live — In most parts of the world, benzodiazepines are only considered legal if given a prescription by a medical doctor.
- 📞 Know where to go if you need help — Help is available for benzodiazepine addiction; you just have to ask for it. Look up “addiction hotline” for more information about where you live. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
Nitrazepam Drug Interactions
As previously discussed, nitrazepam should never be coadministered with compounds that depress the CNS. But, as the metabolism of nitrazepam is not CYP-mediated, there is no significant risk when it comes to drugs that can either inhibit or induce enzymes belonging to the CYP family.
Nitrazepam Contraindications
Canadian health authorities have identified the following contraindications for nitrazepam:
- Known hypersensitivity to benzodiazepines
- Severe impairment of respiratory function
- Significant sleep apnea syndrome
- Myasthenia Gravis
- Severe hepatic insufficiency
- Nitrazepam is contraindicated in children when used as a hypnotic

Nitrazepam Dosage
As a prescription medication, the proper dosage of nitrazepam is something that a doctor should determine on a case-by-case basis. However, it’s still a good idea to learn the normal dosing ranges.
According to Canadian health authorities, the average dosing regimen for nitrazepam is between 2.5 and 10 mg per day — usually taken before bed.
The optimal dose of nitrazepam can vary substantially according to tolerance, underlying conditions, treatment goals, age, and more.
Never attempt to take benzodiazepines without first consulting with your doctor.
Compared to other benzodiazepines, nitrazepam is considered roughly average. It has a similar potency to diazepam (Valium) but is much weaker than drugs like alprazolam (Xanax), clonazepam (Klonopin), and brotizolam.
Estimated Equivalency to Other Common Benzodiaepines
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
Similar Benzodiazepines
Interested in learning what benzodiazepines have comparable characteristics to nitrazepam? This section will list some examples.
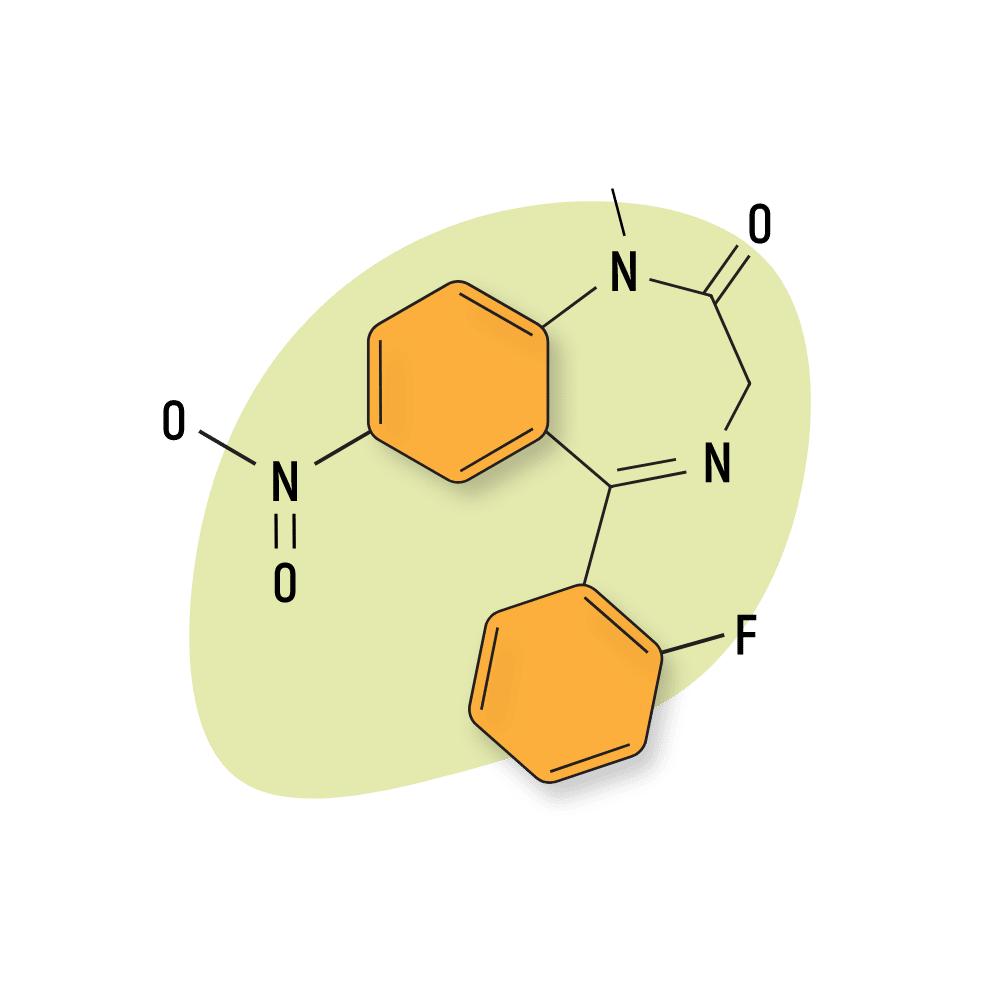
Flunitrazepam
In structural terms, flunitrazepam has a lot of similarities to nitrazepam. They’re essentially the same compound, except that flunitrazepam has a fluoro group at position two and a methyl group at position one. This difference means that flunitrazepam is considerably more potent, but they’re quite similar in most respects.
Clonazepam
Clonazepam (Klonopin) is another nitrobenzodiazepine and one of the market’s most commercially successful benzodiazepines. Both clonazepam and nitrazepam have intermediate half-lives, but clonazepam is far more potent.
Natural Alternatives to Benzodiazepines
Here are some natural alternatives to benzodiazepines that can offer comparable benefits but with fewer side effects!
L-Theanine
L-Theanine, a natural compound found in green and black tea, can interact with two different types of neurotransmitters, glutamate, and GABA, to produce a depressive effect on the CNS that is comparable to that of benzodiazepines [10]. However, it should be noted that the effect is less potent than that of a pharmacological benzodiazepine.
Kratom
Kratom is another natural compound with a reduced side effects profile but has a much wider range of effects than L-Theanine. In low doses, kratom acts like a stimulant and a euphoric, similarly to coffee, but the higher the dose, the more anxiolytic and sedative its properties become [11].

Nitrazepam FAQs
Does nitrazepam have clinically active metabolites?
No, the metabolic byproducts of nitrazepam, 7-aminonitrazepam, and 7-acetamidonitrazepam are not pharmacologically active.
What formulations is nitrazepam available in?
Nitrazepam is available in either 5 or 10 mg oral tablets.
Is nitrazepam well absorbed in the body?
The absorption of nitrazepam from the gastrointestinal tract is fairly rapid (Tmax ranging from 0.5 to 7 hours). The bioavailability after oral intake averages about 80%. Maximum plasma concentrations after a single 5mg dose are of the order of 40ng/ml. As a lipophilic drug, nitrazepam is distributed rapidly in the body.
References
- Kangas, L., & Breimer, D. D. (1981). Clinical pharmacokinetics of nitrazepam. Clinical Pharmacokinetics, 6(5), 346-366.
- Skerritt, J. H., & Johnston, G. A. (1983). Enhancement of GABA binding by benzodiazepines and related anxiolytics. European journal of pharmacology, 89(3-4), 193-198.
- Vgontzas, A. N., Kales, A., & Bixler, E. O. (1995). Benzodiazepine side effects: role of pharmacokinetics and pharmacodynamics. Pharmacology, 51(4), 205-223.
- Belzung, C., Misslin, R., & Vogel, E. (1989). Behavioural effects of the benzodiazepine receptor partial agonist RO 16-6028 in mice. Psychopharmacology, 97(3), 388-391.
- Nowakowska, E., & Chodera, A. (1991). Studies on the involvement of opioid mechanism in the locomotor effects of benzodiazepines in rats. Pharmacology Biochemistry and Behavior, 38(2), 265-266.
- TOMONO, S., & KURIYAMA, K. (1985). Effect of 450191-S, a 1H-1, 2, 4-triazolyl benzophenone derivative, on cerebral content of neuroactive amino acids. The Japanese Journal of Pharmacology, 39(4), 558-561.
- Krause, L., & Shuster, S. (1983). Mechanism of action of antipruritic drugs. Br Med J (Clin Res Ed), 287(6400), 1199-1200.
- Christensen, P., Lolk, A., Gram, L. F., & Kragh-Sørensen, P. (1992). Benzodiazepine-induced sedation and cortisol suppression. Psychopharmacology, 106(4), 511-516.
- Riss, J., Cloyd, J., Gates, J., & Collins, S. (2008). Benzodiazepines in epilepsy: pharmacology and pharmacokinetics. Acta neurologica scandinavica, 118(2), 69-86.
- Nathan, P. J., Lu, K., Gray, M., & Oliver, C. (2006). The neuropharmacology of L-theanine (N-ethyl-L-glutamine), a possible neuroprotective and cognitive enhancing agent. Journal of Herbal Pharmacotherapy, 6(2), 21-30.
- Eastlack, S. C., Cornett, E. M., & Kaye, A. D. (2020). Kratom—Pharmacology, clinical implications, and outlook: a comprehensive review. Pain and therapy, 9(1), 55-69.