Bromazolam Fact Sheet: Effects, Safety, and Alternatives
2 little information + 2 many variables = a 4-midable benzo deserving respect… 😒 You’re right. That was too much. No more puns.
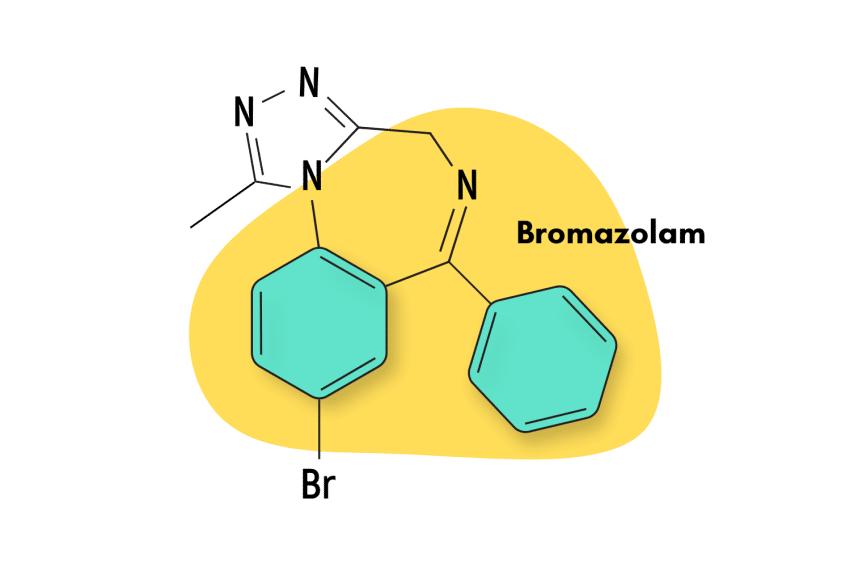
Bromazolam is a designer benzodiazepine that is not approved for medical use. This article will delve into bromazolam’s specifics, safety profile, and other alternatives.
What Is Bromazolam?
Bromazolam is a benzodiazepine derivative that was first synthesized in 1976 but was never marketed. It is not available as a prescription medication as it has not been approved for medical use yet.
Bromazolam was first discovered in a 0.74-gram sample of a yellow powder confiscated by Swedish Customs in Stockholm on August 3rd, 2016.
Bromazolam Specifications
| Status | Research chemical |
| Common Dosage | 1-2 mg |
| PubChem ID | 12562546 |
| CAS# | 71368-80-4 |
| IUPAC name | 8-bromo-1-methyl-6-phenyl-4H-[1,2,4]triazolo[4,3-a][1,4]benzodiazepine |
| Other names | Bromazola; bromazolon; bromazolam; 71368-80-four |
Metabolism
Bromazolam is primarily metabolized in the liver by the cytochrome P450 (CYP450) enzyme complex, including CYP3A4.
Duration of Action
Bromazolam has an onset of action of 15 to 45 minutes following oral intake. Its effect lasts from 5 to 8 hours, while after-effects may last from 1 to 12 hours [1].
What Is the Average Dose of Bromazolam?
The common oral dose of bromazolam is 1-2 mg. Bromazolam may exert its effects at doses as low as 0.5-1.0 mg, while some patients may require higher doses of up to 2-4 mg [1].

Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Bromazolam Work?
Bromazolam exerts its effects by modulating the actions of gamma-aminobutyric acid (GABA), the principal inhibitory neurotransmitter in the central nervous system (CNS). GABA produces its effects by binding to the GABA receptors on neuronal membranes, thus initiating a chain of events. Three types of GABA receptors are known, namely A, B, and C. GABA-A receptors are ligand-gated chloride ion channels comprising five subunits: one γ subunit, two β subunits, and two α subunits [4].
The binding of GABA to GABA A receptors results in the opening of chloride ion channels, resulting in an influx of chloride ions into the neuron. This induces neuron hyperpolarization, thereby decreasing neuronal excitation [3].
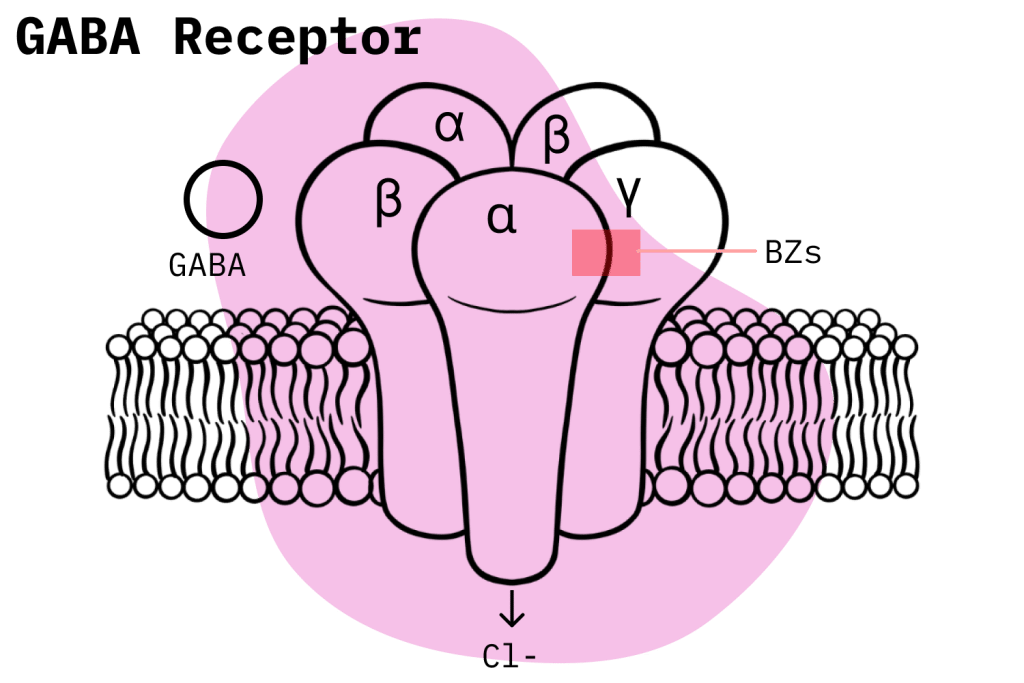
Benzodiazepines bind to a specific pocketed site between the γ and α subunits of GABA A receptors. This binding results in a conformational change of the GABA receptor, which increases the affinity of the receptor to GABA [5]. The ultimate pharmacological response is sedation, anxiolysis, hypnosis, skeletal muscle relaxation, and anticonvulsant activity.
Based on the subunits, the GABA-A receptor has several subtypes. Different benzodiazepines bind with different affinities to these receptor subtypes, displaying various effects. Bromazolam particularly has an affinity for the subtypes α1, α2, and α5 [6].
Is Bromazolam Safe? Risks & Side Effects
Bromazolam is a relatively novel benzodiazepine, and information regarding this drug is deduced mostly from user reports and case studies. Clinical data on bromazolam is, therefore, quite limited.
Prolonged use of bromazolam may lead to physical and psychological dependence, while abrupt drug discontinuation may result in unpleasant withdrawal symptoms. Tolerance may develop with subsequent drug use, ultimately requiring continuous dose increments. Drug-seeking behavior is also likely [1].
Acute intoxication with bromazolam may result in marked respiratory and central nervous system depression. Bromazolam overdose is rarely lethal when taken alone. However, serious respiratory and central nervous system depression may occur if bromazolam is abused with other central nervous system-depressing drugs.

Designer benzodiazepines are commonly abused street drugs. Since bromazolam has not been FDA-approved for human use, its complete pharmacological profile is largely unknown. Concomitant use of bromazolam with other new psychoactive substances (NPS) or opioids, such as fentanyl, may cause significant CNS depression leading to hospitalizations and fatalities.
To date, bromazolam has been found in more than 250 toxicology cases submitted to NMS Labs in the USA, including both antemortem and postmortem investigations. Bromazolam has also been found in counterfeit benzodiazepine preparations tested at the CFSRE (Center for Forensic Science Research and Education), USA [7]. Hence, further research and regulation of such drugs are required.
Common Side Effects
Some common side effects of bromazolam include:
- Dizziness
- Frequent urination
- Impaired memory and cognition
- Increased salivation
- Lethargy
- Light-headedness
- Loss of balance and coordination
- Loss of libido
- Low mood
- Muscle weakness
- Sleep disturbances, including vivid dream
Serious side effects of bromazolam include:
- Allergy and/or anaphylaxis (skin rash, itching, the appearance of hives, swelling of lips, tongue, and face, cold/clammy skin, difficulty in breathing)
- Bleeding from the nose (epistaxis) and/or gums
- Depressed mood with or without suicidal thoughts
- Difficulty in breathing with short and shallow breaths
- Loss of memory (amnesia) and confusion
- Palpitations
- Perception of something that is not present (hallucinations) and/or false belief (delusions)
- Swelling of the lips
- Yellowish discoloration of eyes and/or skin

Harm Reduction
Bromazolam is a research drug that has not been approved by the FDA for clinical use. Bromazolam should not be consumed or purchased from unreliable and unverified sources since the exact composition of the provided substance is unknown. Use of bromazolam with other CNS depressants, such as alcohol and opioids, is not advisable.
- 🥣 Do not mix — Mixing benzodiazepines with other CNS depressants (alcohol, GHB, phenibut, barbiturates, opiates) causes synergistic CNS depression, which may be fatal.
- ⏳ Drug holiday — Benzodiazepines should not be used continuously for more than 1-3 weeks and should always be used under medical supervision.
- 🥄 Take the medicine as advised/prescribed — Benzodiazepines may produce marked CNS sedation in some patients, even at low doses. Many factors determine how you respond to the drug, including gender, age, body weight, use of other medicines and supplements, and functional status of other organs.
- 👨⚕️ Ask your doctor or pharmacist for contraindications — Most benzodiazepines may not be suitable for use in children, the elderly, pregnant and breastfeeding women, and individuals with reduced liver and kidney function.
- 🧪 Purchase from licensed hospitals and pharmacies — In case of purchasing benzodiazepines from sources other than licensed hospitals and pharmacies, obtaining the product with a testing kit to confirm identity is recommended.
- 💉 Do not inhale or inject benzodiazepines intended for oral use — Administering benzodiazepines via unapproved routes of administration may have unpredictable effects on their properties and is not recommended.
- 🌧️ Recognize signs of addiction — If not taking the drug makes you sick with headache, nausea, vomiting, diarrhea, abdominal cramps, and/or sweating, and these symptoms improve after drug administration, seek medical care immediately. You may be developing an addiction to the drug, which may increase in severity with prolonged unsupervised drug use.
- ⚖️ Understand local laws — Benzodiazepines are prescription medicines in most countries, and unauthorized purchase, use, and possession may be illegal.
- 📞 Know where to find help — Most countries have assistance programs for benzodiazepine addiction. Seek advice if you believe you need help. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
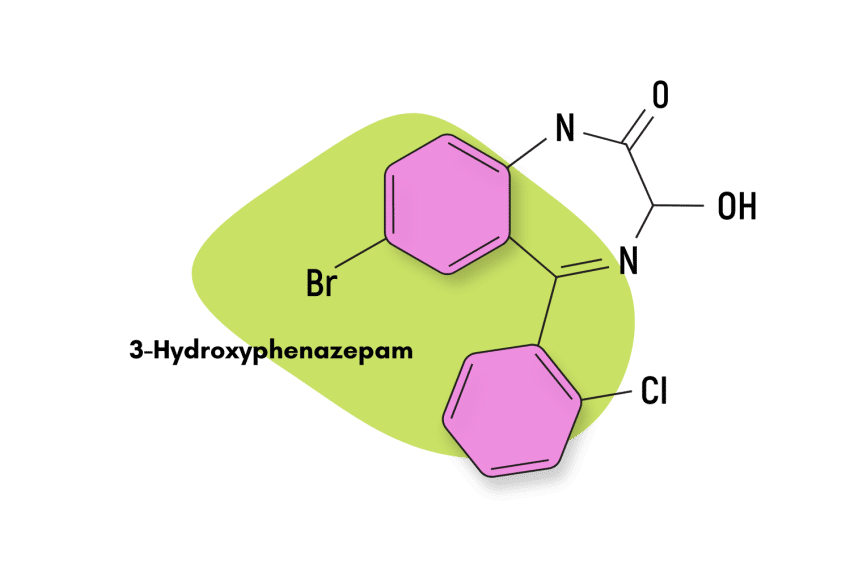
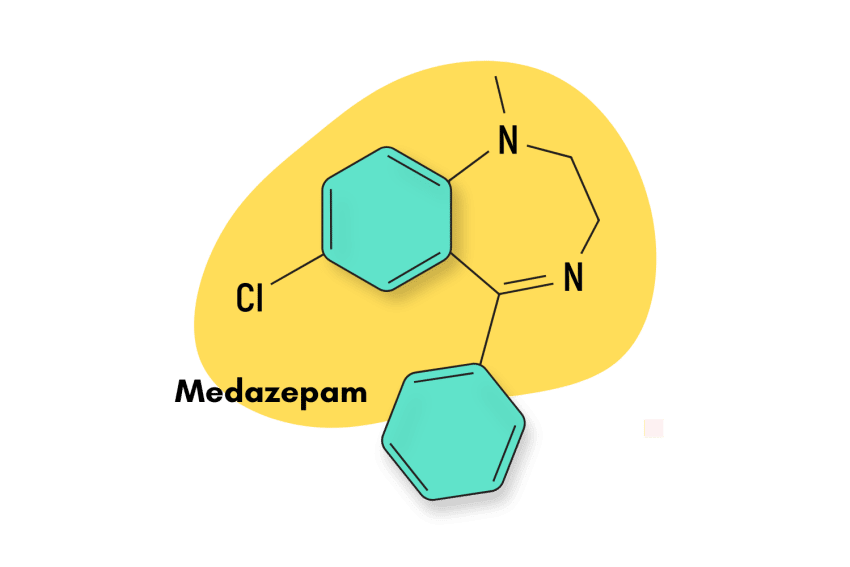
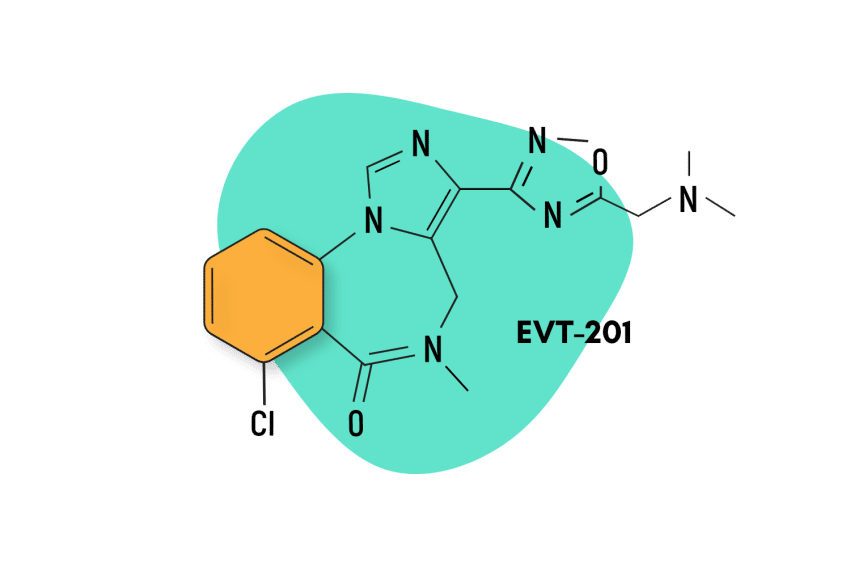
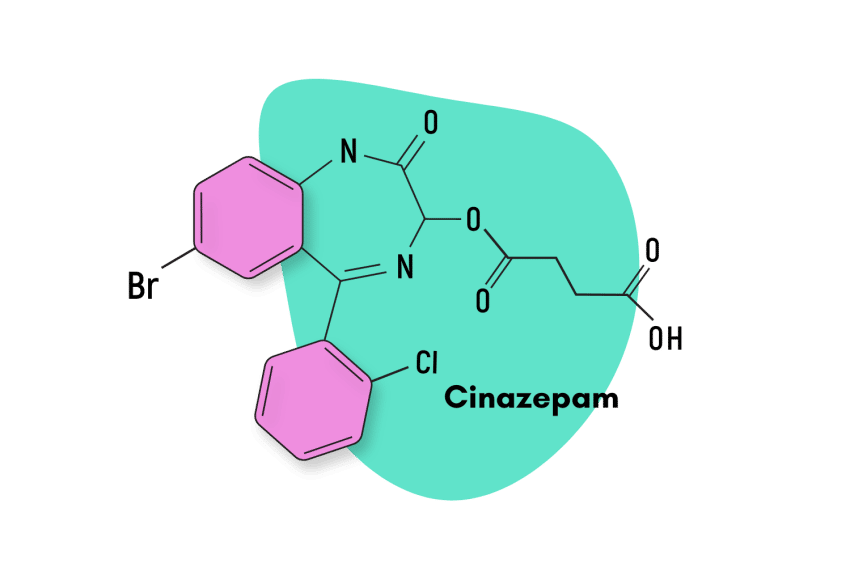
Similar Benzodiazepines
Bromazolam is a short-acting benzodiazepine with a half-life of 6-24 hours. The time for onset of action is 15-45 minutes. Similar benzodiazepines are summarized below.
Bromazolam vs. Other Short-acting Benzodiazepines
| Bromazolam | Alprazolam | Pyrazolam | Flubromazolam | |
| Chemical composition | 1,4-benzodiazepine | Benzodiazepine with a triazole ring attached to its structure | 1,4-benzodiazepine | 1,4-benzodiazepine |
| Route of administration | Oral | Oral | Oral | Oral |
| Onset of action | 15-45 minutes | 15-40 minutes | 10-15 minutes | 20-45 minutes |
| Time to peak concentration | 1-2 hours | 1-2 hours | 1-2 hours | 5 hours |
| Duration of action | 5-8 hours (short-acting) | 5-8 hours (short-acting) | 5-8 hours (short-acting) | 6-12 hours (intermediate-acting) |
| Mechanism of action | GABA-A receptor agonist | GABA-A receptor agonist | GABA-A receptor agonist | GABA-A receptor agonist |
| Medical use | Anxiety disorders, muscle relaxation | Panic disorders, anxiety disorders, insomnia | Anxiety disorders, sedation | Anxiety disorders, insomnia |
Natural Alternatives To Benzodiazepines
Some naturally-occurring compounds have been found to show activity similar to bromazolam by mimicking the action of GABA. However, the evidence regarding their efficacy is poor due to a lack of clinical data. Therefore, always consult your doctor or pharmacist before using any of these alternative medicines.
Natural alternatives to bromazolam include:
1. Kava
Kava (Piper methysticum)is a popular over-the-counter herbal remedy used for insomnia, stress, and anxiety. It is consumed in the form of tea. Kavain is the main active constituent in kava, which works in a fashion similar to benzodiazepines by enhancing the effect of GABA [8].

2. Gotu Kola
Gotu Kola (Centella asiatica) is a herb that has been used to treat anxiety, epilepsy, and depression since antiquity. It is believed that the antiepileptic properties are because of its ability to increase the levels of GABA in the brain [9].
3. Ashwagandha
Ashwagandha is a herb used in traditional medicine for its positive effects on health. In a study, aqueous ashwagandha root extract was given to participants for eight weeks and was found to lower stress and improve quality of life [10].
4. Lavender Essential Oil
Lavender essential oil has been used since ancient times for its anxiolytic properties, which have recently been backed by clinical studies. The two primary active constituents of lavender essential oil are linalool and linalyl acetate.
The combined effect of these constituents may produce an anxiolytic effect by inhibiting voltage-gated calcium ion channels, reducing 5HT1A receptor activity, and increasing parasympathetic tone [11].
5. Valerian Root
Valerian (Valeriana officinalis) is another herb used to treat sleep disorders since ancient times. It has sedative and hypnotic properties and is currently gaining popularity as it is available over the counter. Studies have found the active constituents in valerian root modulate GABA-A receptors allosterically, even facilitating the release of GABA [12].
6. Chamomile
Chamomile is a popular herbal tea used to aid in sleep and anxiety disorders. The exact mechanism of how chamomile produces these effects is currently unknown. However, some studies show that its active principles may modulate the action of such neurotransmitters as GABA, dopamine, serotonin, and noradrenaline [13].

Bromazolam FAQs
Can I be prescribed bromazolam?
Although bromazolam was first synthesized in the 1970s, it has not been approved yet for therapeutic use in the United States and is not available for prescribing [8]. Since most of its properties are unknown, other alternative benzodiazepines are safer for use.
Is bromazolam safe for use?
Safety and other data on bromazolam are largely derived from case studies and user reports, and complete safety information has not been elucidated yet in large-scale clinical trials.
References
- Orsolini, L., Corkery, J. M., Chiappini, S., Guirguis, A., Vento, A., De Berardis, D., … & Schifano, F. (2020). ‘New/Designer Benzodiazepines’: an analysis of the literature and psychonauts’ trip reports. Current neuropharmacology, 18(9), 809-837.
- Canton, H. (2021). United Nations Office on Drugs and Crime—UNODC. In The Europa Directory of International Organizations 2021 (pp. 240-244). Routledge.
- DeVane, C. L., Ware, M. R., & Lydiard, R. B. (1991). Pharmacokinetics, pharmacodynamics, and treatment issues of benzodiazepines: alprazolam, adinazolam, and clonazepam. Psychopharmacology bulletin, 27(4), 463-473.
- Jenner, P., Pratt, J. A., & Marsden, C. D. (1986). Mechanism of action of clonazepam in myoclonus in relation to effects on GABA and 5-HT. Advances in neurology, 43, 629-643.
- Griffin, C. E., 3rd, Kaye, A. M., Bueno, F. R., & Kaye, A. D. (2013). Benzodiazepine pharmacology and central nervous system-mediated effects. The Ochsner journal, 13(2), 214–223.
- Clayton, T., Poe, M. M., Rallapalli, S., Biawat, P., Savić, M. M., Rowlett, J. K., … & Cook, J. M. (2015). A review of the updated pharmacophore for the alpha 5 GABA (A) benzodiazepine receptor model. International journal of medicinal chemistry, 2015.
- Bromazolam Prevalence Surging Across the United States Driven In Part by Increasing Detections Alongside Fentanyl. NPS Discovery. (n.d.). Retrieved September 11, 2022, from https://www.npsdiscovery.org/
- Chua, H. C., Christensen, E. T., Hoestgaard-Jensen, K., Hartiadi, L. Y., Ramzan, I., Jensen, A. A., … & Chebib, M. (2016). Kavain, the major constituent of the anxiolytic kava extract, potentiates GABAA receptors: functional characteristics and molecular mechanism. PLoS One, 11(6), e0157700.
- Gohil, K. J., Patel, J. A., & Gajjar, A. K. (2010). Pharmacological review on Centella asiatica: a potential herbal cure-all. Indian journal of pharmaceutical sciences, 72(5), 546.
- Salve, J., Pate, S., Debnath, K., & Langade, D. (2019). Adaptogenic and anxiolytic effects of ashwagandha root extract in healthy adults: a double-blind, randomized, placebo-controlled clinical study. Cureus, 11(12).
- Malcolm, B. J., & Tallian, K. (2017). Essential oil of lavender in anxiety disorders: ready for prime time?. Mental Health Clinician, 7(4), 147-155.
- Shinjyo, N., Waddell, G., & Green, J. (2020). Valerian root in treating sleep problems and associated disorders—A systematic review and meta-analysis. Journal of Evidence-Based Integrative Medicine, 25, 2515690X20967323.
- Mao, J. J., Li, Q. S., Soeller, I., Rockwell, K., Xie, S. X., & Amsterdam, J. D. (2014). Long-term chamomile therapy of generalized anxiety disorder: A study protocol for a randomized, double-blind, placebo-controlled trial. Journal of clinical trials, 4(5).