Clonazepam (Klonopin): The Euphoric Benzodiazepine
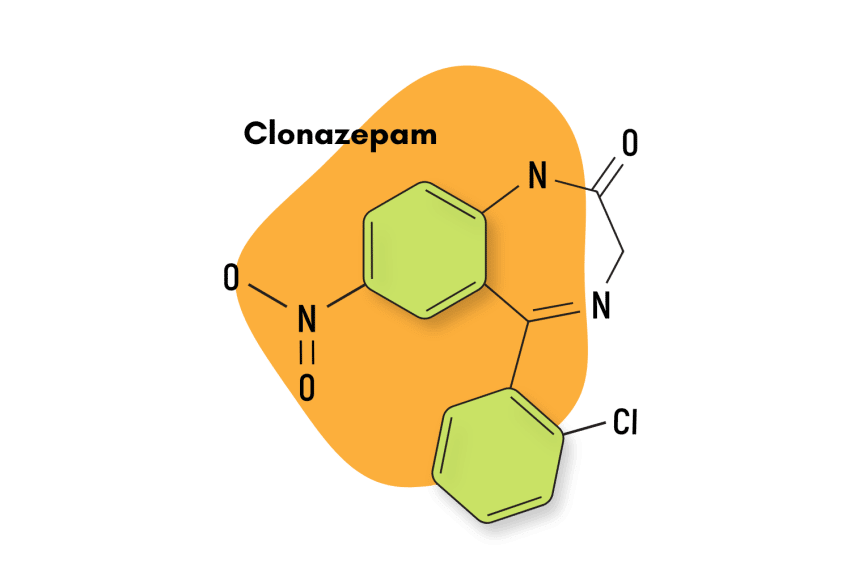
Clonazepam (Klonopin) is one of the most popular members of the benzodiazepine class of drugs. It’s closely related to diazepam (Valium) and chlordiazepoxide (Librium).
Klonopin has remained one of the most commonly prescribed medications in the US for over 20 years. As of 2019, Klonopin was listed as the 46th most prescribed medication in the US.
The drug is habit-forming, which means that misuse of clonazepam can cause addiction. It’s thought to be more euphoric and less sedative than other drugs of the same class. Some recreational users refer to this drug as the “MDMA of the benzo world.”
A large number of young people abuse clonazepam for its euphoric properties. Studies support the idea that long-term use of Klonopin leads to issues with cognition (learning and memory), immune health, and rebound insomnia and anxiety.
Clonazepam was first patented in 1960 by Roche and later approved by the Food and Drug Administration (FDA) in 1975. The patent for clonazepam expired long ago, and there are now many generic versions of the drug sold under different names [1].
Clonazepam Specs
IUPAC Name: 5-(2-chlorophenyl)-7-nitro-1,3-dihydro-1,4-benzodiazepine-2-one
Other Names: Rivatril, Rivotril, Klonopin, Iktorivil, Paxam
Metabolism
Clonazepam is primarily metabolized into inactive metabolites by the cytochrome P450 enzymes, including the CYP3A4 enzyme. Because it is lipid-soluble, it can easily cross the placenta and the blood-brain barrier [2].
Duration of Effects
Intermediate-Acting (9.5–50 hours). The half-life of clonazepam ranges between 19 to 60 hours. It usually reaches peak concentrations within 1 to 2 hours of consumption [2].

What is the Dose of Clonazepam?
The oral tablet is available in the following doses: 0.5 mg, 1 mg, and 2 mg. The medicine is also available in the form of orally disintegrating tablets in the following doses: 0.125 mg, 0.25, 0.5 mg, 1 mg, and 2 mg.
The usual starting dose for panic disorder is 0.25 mg, taken twice daily, and 0.5 mg is taken three times per day for seizures.
Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Clonazepam Work?
Gamma-Aminobutyric acid (GABA) is the major inhibitory neurotransmitter in the body. GABA binds to the GABA receptors at the neuronal end. There are three known GABA receptors — A, B, and C. GABA-A receptors open the chloride channel, causing neuronal hyperpolarization and less excitation of neurons [3].
Benzodiazepines like clonazepam bind to the GABA-A receptors and enhance their sensitivity to endogenous (naturally occurring) GABA [4]. This results in a “dulling” of electrical activity in the brain, leading to reduced feelings of anxiety, slowed thoughts, and sedation.
This activity also results in the relaxation of skeletal muscles. This is because benzodiazepine receptor-associated GABA-A receptors exist peripherally and in the central nervous system (CNS) [5].
The GABA receptors have 1 γ (gamma) subunit, 2 β (beta) subunits, and 2 α (alpha) subunits. The benzodiazepines bind at a specific space between the γ and α subunits. The binding of benzodiazepines to the pocketed space between the γ and α subunits results in a conformational change of the GABA receptor, resulting in increased receptor affinity to GABA [6].
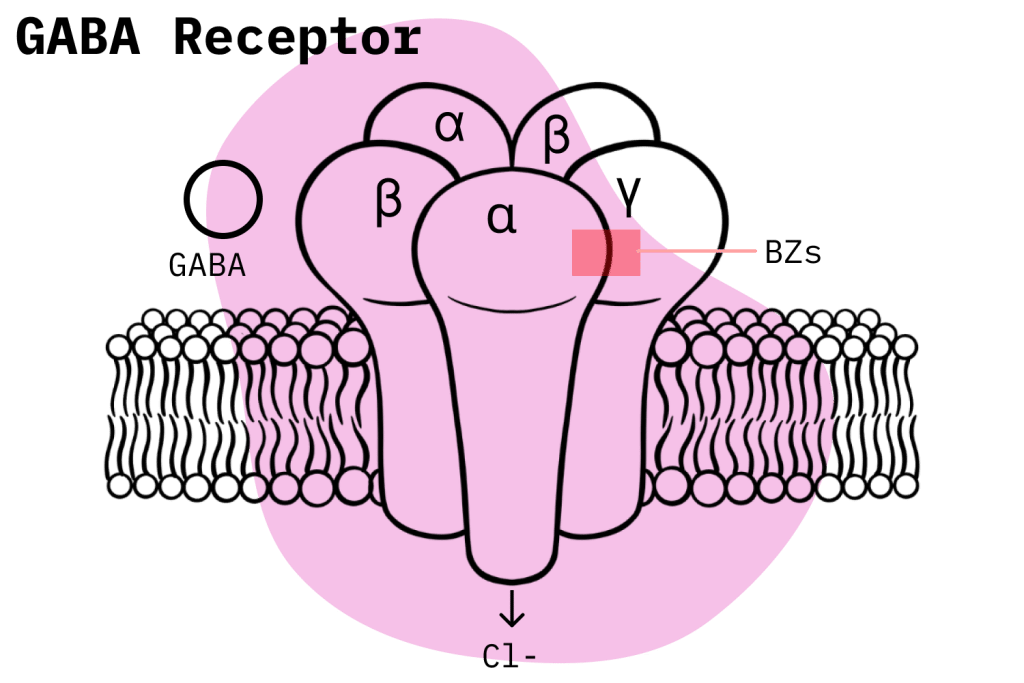
The GABA-A receptor is further classified into several subtypes based on its subunits. The BZ1 receptor has the α1 isoform, whereas the BZ2 receptor contains the α2 isoform. The BZ1 receptor mediates the sedative effects of benzodiazepines because it is found abundantly in the cerebellum, cortex, and thalamus. The BZ2 is responsible for the anxiolytic effects of benzodiazepines as it is present in high concentrations in the dorsal horn of the spinal cord, the motor neurons, and the limbic system [6].
Different benzodiazepines act with varying affinity to the various receptor subtypes. This is why different benzodiazepines do not have similar effects. Clonazepam binds to both α1 and α2 isoforms with equal affinity [8].
Is Clonazepam Safe? Risks & Side Effects
Clonazepam should be strictly used only under the prescription of a doctor. The drug can be habit-forming and can result in physical dependence. If you stop the drug abruptly on your own, there may be unpleasant symptoms of benzodiazepine withdrawal, such as abdominal cramps, anxiety, sweating, tremors, blurred vision, concentration problems, and dizziness.
Additionally, clonazepam intake with certain medications can cause breathing problems, sedation, or coma, which can even be life-threatening.
Clonazepam is a safe drug if used under your doctor’s prescription and by informing your prescriber about your health condition and all the medicines you are taking.
However, there are specific side effects that you might experience despite following all the instructions. The side effects can range from mild to severe. The mild form of these side effects is more common.
Common Side Effects Of Clonazepam
- Blurring of vision
- Dizziness
- Drowsiness
- Decreased sex drive
- Frequent urination
- Increased salivation
- Lightheadedness
- Low mood
- Muscle weakness
- Problems with thinking and memory
- Sleep disturbance with vivid dreams
- Unsteadiness and problems with balance
Rarer but more serious side effects of clonazepam include:
- Breathing problems (usually seen as short and shallow breathing while unconscious)
- Yellowish discoloration of eyes or skin. This is a sign of problems with the liver.
- Amnesia (loss of memory) and confusion
- Seeing or hearing things that are not there (hallucination), false beliefs (delusions)
- Signs of heart problems such as swelling of limbs, racing heartbeat and feeling tired.
- Bleeding problems such as nasal bleeding
- Depressed mood or thoughts of harming yourself
- Signs of anaphylaxis such as rashes, itching, hives, swelling of lips, tongue, or face, hoarseness of voice, difficulty in breathing, and confusion

Harm Reduction: Clonazepam
The main concerns with clonazolam are the risk of potentiating overdose on other drugs or medications (especially other sedatives like alcohol, opiates, phenibut, or GHB) and abuse/addiction.
Here are some simple tips to follow to minimize your risk when taking powerful benzodiazepine drugs like clonazepam:
- 🥣 Don’t mix — Mixing benzodiazepines with other depressants (alcohol, GHB, phenibut, barbiturates, opiates) can be fatal.
- ⏳ Take frequent breaks or plan for a short treatment span — Benzodiazepines can form dependence quickly, so it’s important to stop using the drug periodically.
- 🥄 Always stick to the proper dose — The dosage of benzos can vary substantially. Some drugs require 20 or 30 mg; others can be fatal in doses as low as 3 mg.
- 💊 Be aware of contraindications — Benzodiazepines are significantly more dangerous in older people or those with certain medical conditions.
- 🧪 Test your drugs — If ordering benzos from unregistered vendors (online or street vendors), order a benzo test kit to ensure your pills contain what you think they do.
- 💉 Never snort or inject benzos — Not only does this provide no advantage, but it’s also extremely dangerous. Benzos should be taken orally.
- 🌧 Recognize the signs of addiction — Early warning signs are feeling like you’re not “yourself” without the drug or hiding your habits from loved ones.
- ⚖️ Understand the laws where you live — In most parts of the world, benzodiazepines are only considered legal if given a prescription by a medical doctor.
- 📞 Know where to go if you need help — Help is available for benzodiazepine addiction; you just have to ask for it. Look up “addiction hotline” for more information about where you live. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
Reducing The Risk Of Drug Dependence
Clonazepam is not usually addictive if you take it for a short duration, such as 2 to 4 weeks. If you take clonazepam for longer, the dose will need to be reduced gradually before stopping intake completely. Take the dose as prescribed by your doctor.
Restrict Certain Activities While Taking The Drug
Do not drive or operate heavy machinery when you are taking clonazepam. Also, drinking alcohol should be avoided while taking clonazepam. It can make you feel very sleepy and have difficulty waking up.

Clonazepam Drug Interactions
It would be best if you inform your doctor about all the medications that you are taking, especially medicines such as other benzodiazepines, sedatives, hypnotics, phenobarbital, phenytoin, and certain SSRIs like fluvoxamine, antihistamines, and drugs that affect the metabolism of benzodiazepines like antibiotics, antifungals and protease inhibitors.
Do Not Take The Drug If You Suffer From Certain Medical Conditions
You must inform your doctor if you have any health conditions, as clonazepam may worsen them. Clonazepam should be avoided:
- Any major surgeries
- Any psychiatric condition
- Chronic lung disease
- Glaucoma
- Kidney disease
- Liver disease
- Pregnancy, breastfeeding women, or those planning to become pregnant.
Similar Benzodiazepine Alternatives
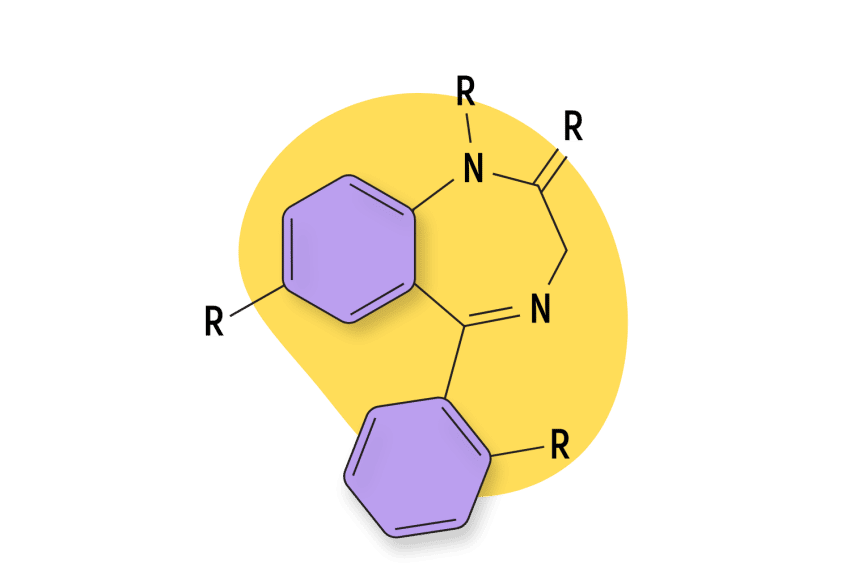
Clonazepam is a long-acting 1,4-benzodiazepine with a half-life averaging 40 hours. Its time for onset of action is about 1 hour. Like other drugs falling under the benzodiazepine class, it is a potent central nervous system depressant with the potential for dependence.
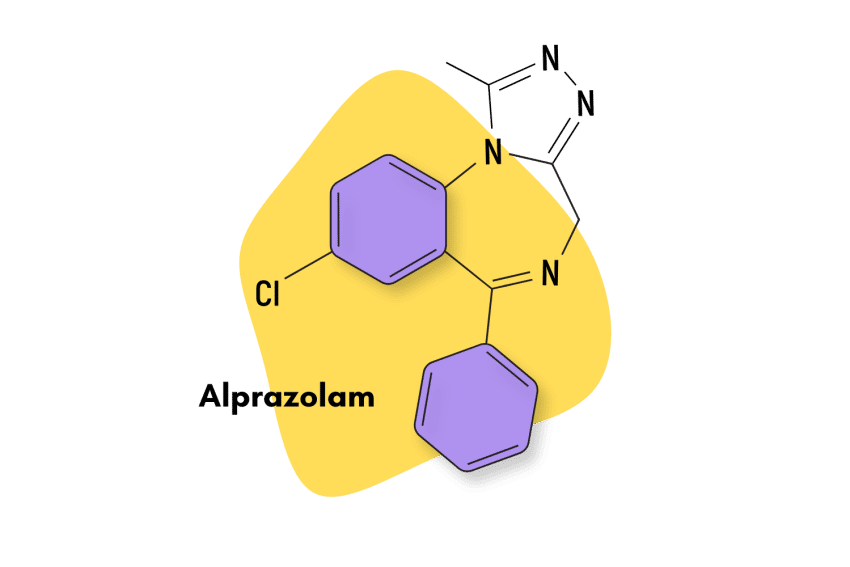
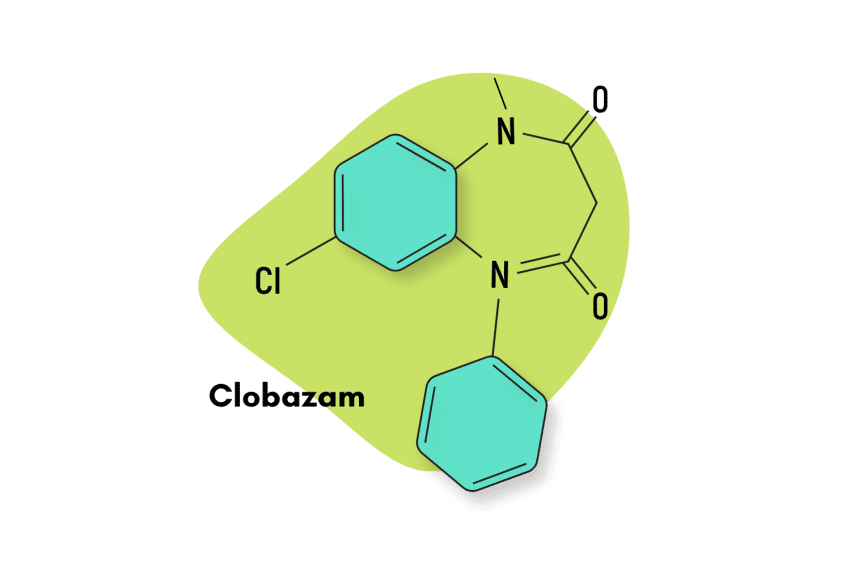
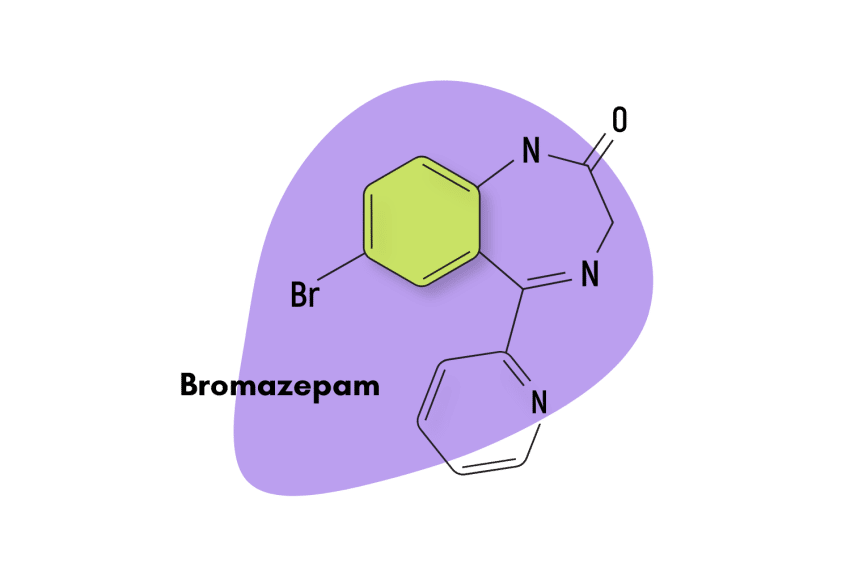
Other benzodiazepines having similar effect profiles as clonazepam include alprazolam (Xanax), bromazepam (Lectopam), diazepam (Valium), chlordiazepoxide (Librium), and lorazepam (Ativan).
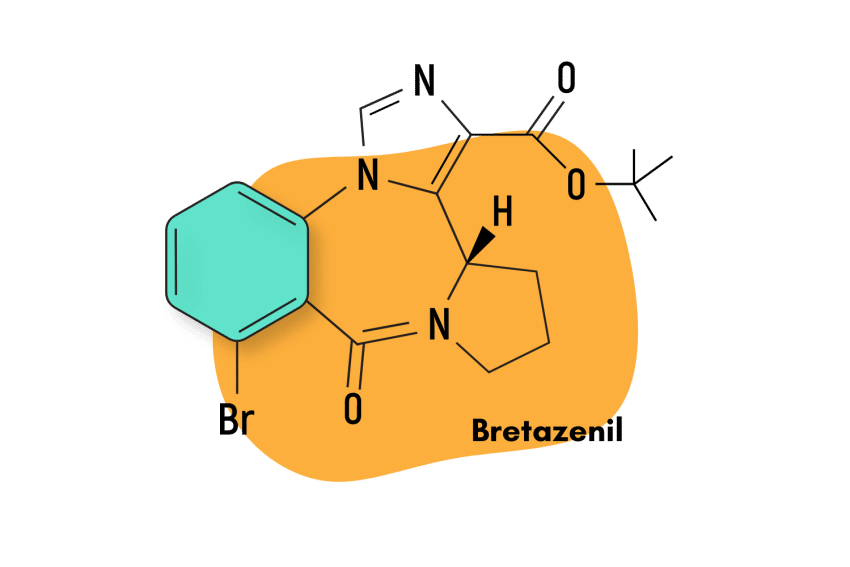
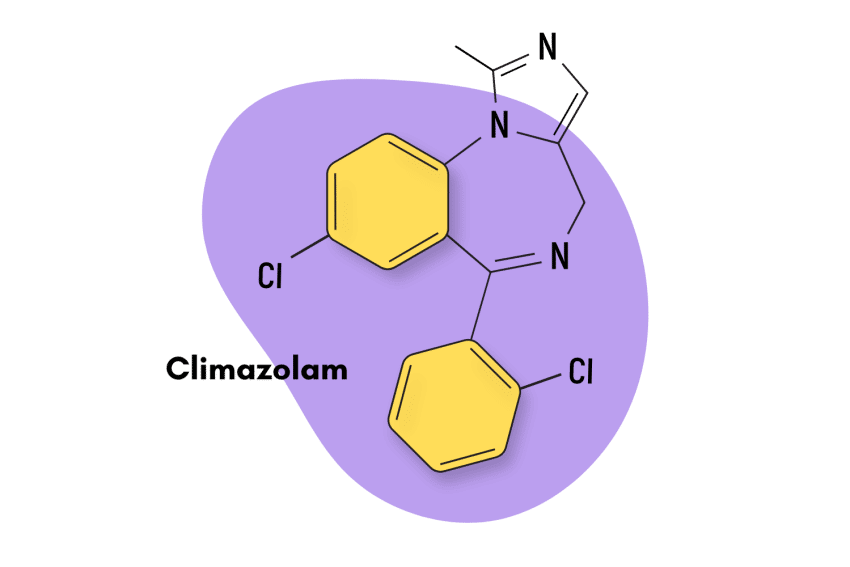
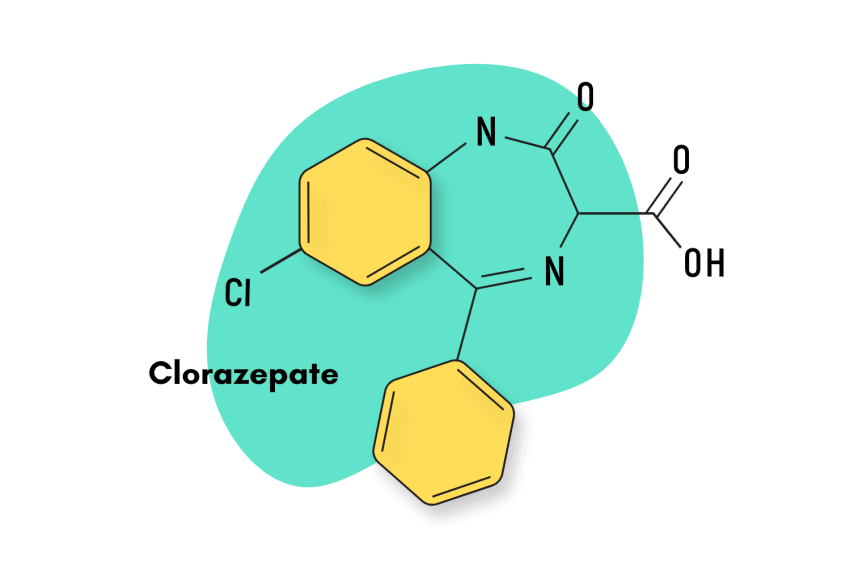
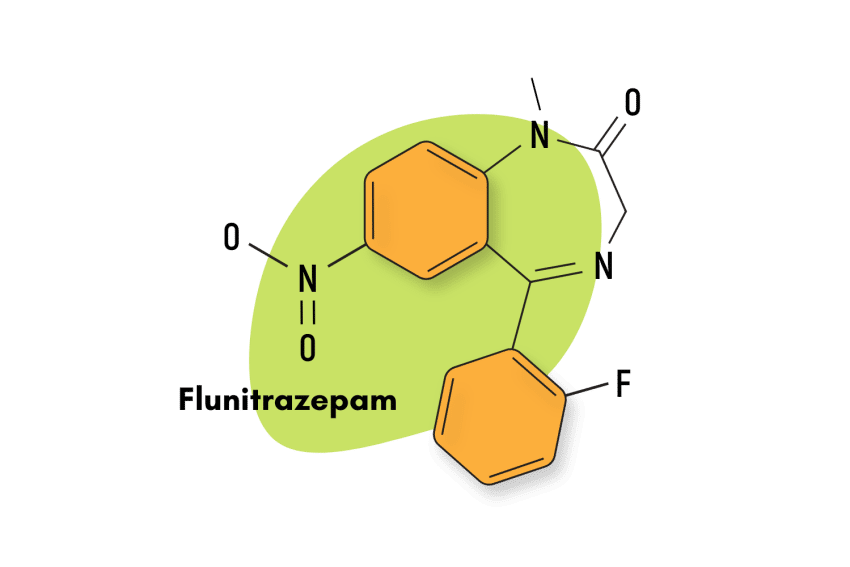
Some of the more obscure, but similar benzodiazepine alternatives include etizolam, metaclazepam (Talis), bretazenil, and oxazolam.
Clonazepam vs. Other Short To Intermediate-Acting Benzodiazepines
| Clonazepam | Alprazolam | Bromazepam | Diazepam | Chlordiazepoxide | |
| Chemical composition | 1,4-benzodiazepine | Benzodiazepine with a triazole ring attached to its structure | 1,4-benzodiazepine | 1,4-benzodiazepine | 1,4-benzodiazepine |
| Route of administration | Oral | Oral | Oral | IV, IM | Oral, IV |
| Onset of action | 1 hour | 20 to 60 minutes | 60 minutes | 15 to 60 minutes | 1 to 2 hours (oral) |
| Peak concentration | 1 to 2 hours | 1 to 2 hours | 1 to 4 hours | 1 to 1.5 hours | 2 hours |
| Duration of effects | Intermediate-acting (18 to 50 hours) | Short-acting (6 to 27 hours) | Intermediate-acting (8 to 19 hours) | Long-acting (20 to 80 hours) | Long-acting (36 to 200 hours) |
| Mechanism of action | GABA-A receptor agonist | GABA-A receptor agonist | GABA-A receptor agonist | GABA-A receptor agonist | GABA-A receptor agonist |
| Medical Uses | Panic disorders, seizures, anxiety | Panic disorders, anxiety disorders, insomnia | Anxiety disorder, alcohol withdrawal | Seizures, alcohol withdrawal, insomnia, muscle spasms, panic disorder, anxiety disorders | Panic disorders, alcohol withdrawal, anxiety disorders |
Natural Alternatives To Benzodiazepines
A few traditional herbal medicines and nutritional supplements work through mechanisms like benzodiazepines (GABAergic). These plants and nutrients may offer a viable alternative to benzodiazepine medications and are sometimes used to help people wean themselves off after becoming dependent.
However, it’s important to note that none of these recommendations offer the same potency as prescription benzodiazepine drugs. They’re much gentler and therefore carry much lower risk.
With that aside, here are some of the best natural benzodiazepine alternatives to consider:
Kava
Kava (Piper methysticum) is a traditional root plant available as an over-the-counter herbal remedy for anxiety, stress, and insomnia. Its major constituent, kavain, and related kavalactones share a similar mechanism of action on the GABA receptors as benzodiazepines [9].
Kava is consumed as a tea, in capsulated or tincture form, or as a concentrated extract. Like clonazolam, kava is both an anxiolytic and mild euphoriant. It’s often consumed in groups in a similar context to alcohol. The calming and mood-enhancing effects of the plant make it very useful for facilitating conversation.

Gotu Kola
Gotu Kola, or Centella asiatica, is a herb that has been used in the orient for thousands of years as an anxiolytic, antiepileptic, antidepressant, and sedative. It has been hypothesized that its antiepileptic properties are due to its ability to increase the levels of GABA in the cerebrum [10].
Valerian Root
Valerian (Valeriana officinalis L.) is a herb that’s been in use since the first century AD. More recently, it’s been gaining popularity for its hypnotic and sedative properties as an alternative to benzodiazepine drugs.
Studies show that these effects of the valerian root owe themselves to its ability to modulate GABA-A receptors and also increase the release of GABA itself [11].

L-Theanine
L-theanine is an amino acid found in green tea. Green tea is well known for its anxiolytic and calming effects. These effects are largely due to the presence of L-theanine itself.
L-theanine exerts its calming action by increasing the synthesis of GABA and modulating effects on dopamine, serotonin, and norepinephrine.
Unlike other GABA-A receptor modulators, L-theanine does not lead to a slowing of reflexes, drowsiness, cognitive impairment, or memory [12].
GABA Supplements
GABA can also be supplemented to support problems with anxiety or insomnia, but it’s not as effective as you think. This is because orally consumed GABA can barely cross the blood-brain barrier (BBB); most studies suggest that the BBB is impermeable by GABA supplements. So, high doses may be required to achieve desired effects [13].
GABA supplements are better used with other herbs or nutrients on this list. It works synergistically with more active GABAergic substances to provide stronger and longer-lasting effects.
Chamomile
Chamomile (Matricaria chamomilla) is widely used as a herbal tea to treat sleep disorders, anxiety, and gastrointestinal discomfort.
Studies on chamomile suggest that it may modulate the action of neurotransmitters, including GABA, serotonin, dopamine, and noradrenaline [14].
Mugwort
Mugwort, or Artemisia indica, is a well-known herb used for its purported benefits as an antihypertensive, antispasmodic, antiallergic, and bacteriolytic.
Some species of mugwort are also known for their antidepressant and sedative effects. These CNS activities of mugwort may have a similar mechanism as benzodiazepines.
Studies suggest that the fractionated constituents of mugwort bind to the same site as benzodiazepines in the GABA-A receptors [15].

Clonazepam FAQs
How will clonazepam (Klonopin) make me feel?
Clonazepam can make you feel sleepy and relaxed, reducing symptoms of anxiety. Users often report feeling euphoric and experience an increased sense of connection with others. This effect is rare among benzos, which explains why clonazepam is so popular amongst recreational users compared to other, more strictly sedative benzodiazepines.
High doses of clonazepam make users feel tired and groggy. Making decisions or maintaining a conversation can be difficult, and walking or moving around may feel more laborious than usual.
How long does clonazepam take to work?
The immediate effects of clonazepam kick in within about 1 hour. However, some conditions may require several days of clonazepam use before any significant changes are reported.
Will I become addicted after taking clonazepam?
The chance of becoming addicted to clonazepam increases the more often you use it. Once or two doses are unlikely to result in any dependence or addiction, but frequent use over the course of 2 or more weeks carries a high risk of addiction and dependence.
The more often you take clonazepam, the hard it becomes to quit. The side effects of withdrawal can be severe and may require medical intervention to treat effectively.
Do I need to avoid any foods or drinks while taking clonazepam?
The caffeine-containing foods and drinks such as chocolate, tea, coffee, and carbonated beverages can counter the effect of clonazepam and reduce its intended activity.
Similarly, alcohol can potentiate the sedative effect of clonazepam and increases the chances of overdose.
References
- Nderitu, H. E. (2016). Prevalence Of Drug Manipulation To Obtain Prescribed Dose In The Paediatric In-Patient Units In Kenyatta National Hospital (Doctoral dissertation, University of Nairobi).
- Fischer, J., & Ganellin, C. R. (2010). Analog-based drug discovery. Chemistry International–Newsmagazine for IUPAC, 32(4), 12-15.
- DeVane, C. L., Ware, M. R., & Lydiard, R. B. (1991). Pharmacokinetics, pharmacodynamics, and treatment issues of benzodiazepines: alprazolam, adinazolam, and clonazepam. Psychopharmacology bulletin, 27(4), 463-473.
- Jenner, P., Pratt, J. A., & Marsden, C. D. (1986). Mechanism of action of clonazepam in myoclonus in relation to effects on GABA and 5-HT. Advances in neurology, 43, 629-643.
- E Nardi, A., Machado, S., Ferreira Almada, L., Paes, F., Cardoso Silva, A., Jose Marques, R., … & Arias-Carrión, O. (2013). Clonazepam for the treatment of panic disorder. Current Drug Targets, 14(3), 353-364.
- Griffin, C. E., Kaye, A. M., Bueno, F. R., & Kaye, A. D. (2013). Benzodiazepine pharmacology and central nervous system–mediated effects. Ochsner Journal, 13(2), 214-223.
- Jensen, H. S., Nichol, K., Lee, D., & Ebert, B. (2014). Clobazam and Its Active Metabolite N-desmethylclobazam Display Significantly Greater Affinities for a2.
- Tanaka, E. (1999). Clinically significant pharmacokinetic drug interactions with benzodiazepines. Journal of clinical pharmacy and therapeutics, 24(5), 347-355.
- Chua, H. C., Christensen, E. T., Hoestgaard-Jensen, K., Hartiadi, L. Y., Ramzan, I., Jensen, A et al. (2016). Kavain, the major constituent of the anxiolytic kava extract, potentiates GABAA receptors: functional characteristics and molecular mechanism. PLoS One, 11(6), e0157700.
- Gohil, K. J., Patel, J. A., & Gajjar, A. K. (2010). Pharmacological review on Centella asiatica: a potential herbal cure-all. Indian journal of pharmaceutical sciences, 72(5), 546.
- Shinjyo, N., Waddell, G., & Green, J. (2020). Valerian root in treating sleep problems and associated disorders—A systematic review and meta-analysis. Journal of Evidence-Based Integrative Medicine, 25, 2515690X20967323.
- Higashiyama, A., Htay, H. H., Ozeki, M., Juneja, L. R., & Kapoor, M. P. (2011). Effects of l-theanine on attention and reaction time response. Journal of Functional Foods, 3(3), 171-178.
- Boonstra, E., de Kleijn, R., Colzato, L. S., Alkemade, A., Forstmann, B. U., & Nieuwenhuis, S. (2015). Neurotransmitters as food supplements: the effects of GABA on brain and behavior. Frontiers in Psychology, 6, 1520.
- Mao, J. J., Li, Q. S., Soeller, I., Rockwell, K., Xie, S. X., & Amsterdam, J. D. (2014). Long-Term Chamomile Therapy of Generalized Anxiety Disorder: A Study Protocol for a Randomized, Double-Blind, Placebo-Controlled Trial. Journal of clinical trials, 4(5), 188.
- Khan, I., Karim, N., Ahmad, W., Abdelhalim, A., & Chebib, M. (2016). GABA-A Receptor Modulation and Anticonvulsant, Anxiolytic, and Antidepressant Activities of Constituents from Artemisia indica Linn. Evidence-based complementary and alternative medicine : eCAM, 2016, 1215393.