Everything You Need To Know About Alprazolam (Xanax)
Alprazolam (sold commercially as Xanax) is one of the most commonly used benzodiazepine drugs in the world.
We explore how alprazolam works, what risks & side-effects to watch out for, how to stay safe when using it, information on dosage, & much more.
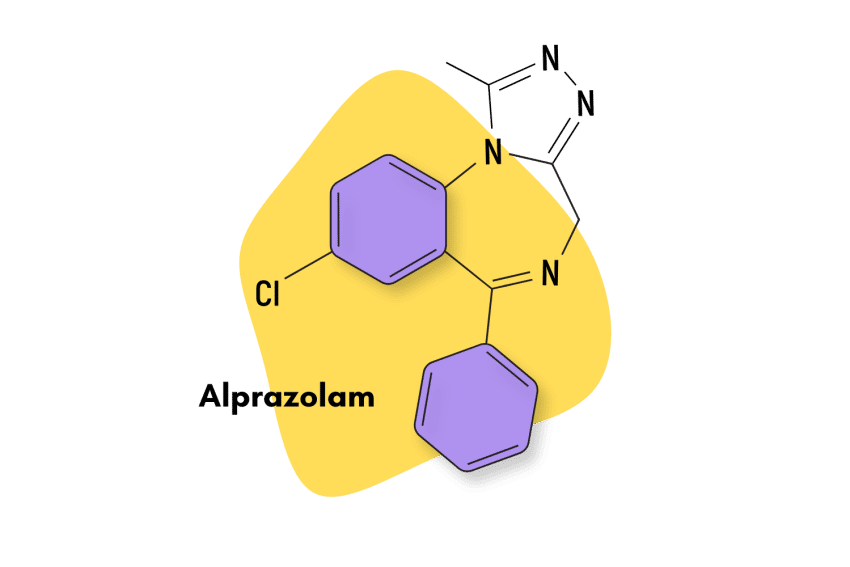
Patented in 1971 and approved for medical use in 1981, alprazolam is a prescription drug of the triazolobenzodiazepine class: a subtype of the larger benzodiazepine family characterized by the inclusion of a triazolo- ring structure.
Compared to other benzodiazepines, the unique characteristics of alprazolam are its fast-acting nature, short half-life, and increased potency.
Alprazolam is far more potent than diazepam, another leading benzodiazepine. Just 1 mg of alprazolam equals roughly 10 mg of diazepam [1].
Know colloquially as “bars,” alprazolam also enjoys a fair amount of renown in the designer drug community as a recreational drug.
Alprazolam Specs
| Status | Approved ✅ |
| Common Dosage | 0.5–1.5 mg |
| PubChem ID | 2118 |
| CAS# | 28981-97-7 |
IUPAC Name: 8-chloro-1-methyl-6-phenyl-4H-[1,2,4]triazolo[4,3-a][1,4]benzodiazepine
Other Names: Xanax, Helex, Xanor, Trankimazin, Onax, Alprox, Misar, Restyl, Solanax, Tafil, Neurol, Frontin, Kalma, Ksalol, Farmapram, & Niravam.
Metabolism: Alprazolam is extensively metabolized in humans, primarily by cytochrome P450 3A4 (CYP3A4), to two major metabolites in the plasma: 4-hydroxyalprazolam and αhydroxyalprazolam.
Duration of Effects: Short-Acting (5-8 hours). The proper dosage of alprazolam lasts around 5 hours and has an elimination half-life of 11-12 hours.

Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Alprazolam Work?
There are meaningful differences between them, but — in general — all benzodiazepines and their subsequent derivatives share the same basic mechanism of action, which gives rise to their anxiolytic, hypnotic, and muscle relaxant properties.
Benzodiazepines exert their effects by slowing down or “inhibiting” activity in the brain and central nervous system (CNS). There are a couple of ways they do this, but the most utilized pathway by far is through their interactions with gamma-aminobutyric acid neurotransmitters, otherwise known as GABA receptors.
GABA receptors are a class of neurotransmitters that cause an inhibitory response in the brain’s neurons.
Benzodiazepines work by potentiating this inhibitory function, usually by binding with the GABA-A transmitter subtype but at a site different from where GABA-A binds: this produces an allosteric effect — a fancy word which means there is increased activity in the receptor [2].
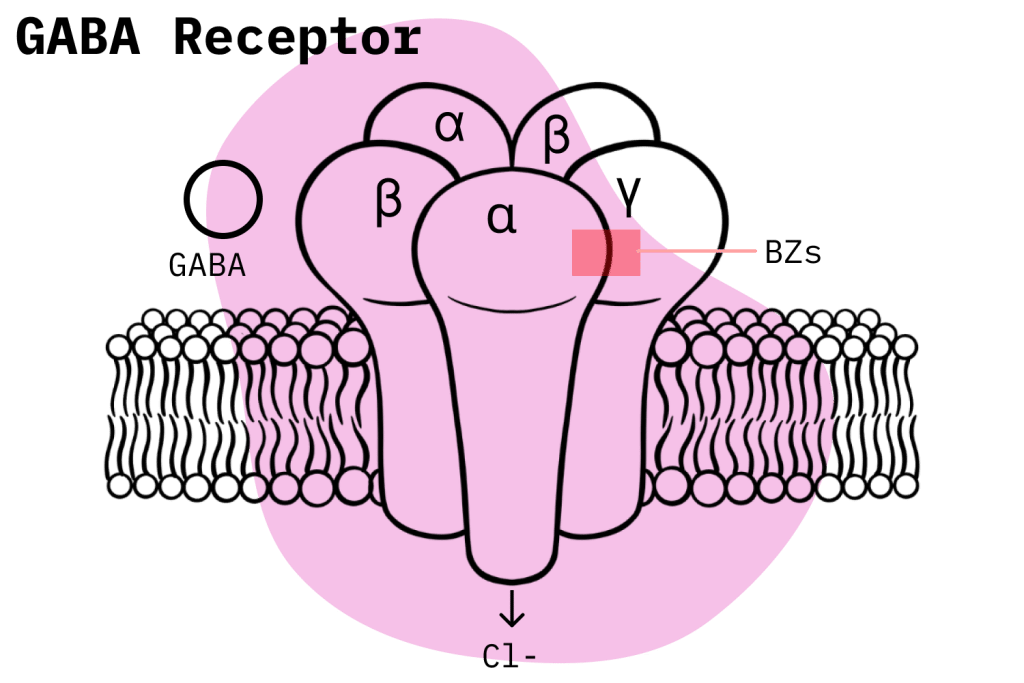
Upon binding, the GABA-A receptor opens its chloride channel, allowing negatively charged chloride ions into the neuron, thus affecting the neuron’s action potential and making it less likely to send electrical impulses throughout the brain and CNS. This inhibitory effect has been shown to reduce anxiety.
Alprazolam targets the GABA-A receptors to produce its effects. However, there are still many unanswered questions about how exactly benzodiazepines bind with GABA-A receptors and go on to produce their allosteric effect.
A lot of the confusion stems from the complex nature of GABA-A receptors. These receptors are made up of a total of 19 subunits. The classification and structure of the subunits is thought to have a determinative effect in the types of effects that are triggered. Essentially, benzodiazepines binding to different subunits trigger different effects [3].
When it comes to alprazolam, we do know that similarly to other classical benzodiazepines, it acts specifically through GABA-A receptors that contain α1/2/3/5, but not α4/6 subunit types. What is less understood, however, are the reasons for this specificity [4].

Is Alprazolam Safe? Risks & Side Effects
Alprazolam is classified by the United States government as a Schedule IV drug, indicating that although it does have accepted medical uses, it still carries the potential for misuse and tolerance, albeit at a lesser risk level than drugs classified as Schedule III.
Statistics show the increased rate of benzodiazepine involvement in overdose deaths is a significant cause for concern. A 2020 survey by the CDC showed that benzodiazepines were involved in 12.290 deaths in the US. Additionally, the NIDA published another study claiming that 16% of overdose deaths involving opioids also had the presence of benzodiazepines.
These trends are alarming but — more specifically — how does alprazolam factor into the larger context?
Studies show that alprazolam is not only the most commonly prescribed benzodiazepine in the United States but also the most common psychotropic medication in the US [1]. Compared to other benzodiazepines, alprazolam has a high potential for misuse.
Based on national emergency department (ED) visit data, alprazolam is the second most common prescription medication and the most common benzodiazepine to be involved in ED visits related to drug misuse (SAMHSA, 2013). This would mean that alprazolam is related to more ED visits than the next three commonly prescribed benzodiazepines (lorazepam, diazepam, and clonazepam).
CDC statistics further show their increased potential for danger and misuse. Between 2003 and 2009, alprazolam had the highest death rate increase of all benzodiazepines and the second highest overall at 234%, compared with 168% for benzodiazepines as a class (CDC, 2011) [1].
Less understood is why alprazolam is more dangerous than other benzodiazepines. It could be that the increased misuse statistics come more as a result of its increased usage relative to other benzodiazepines. Still, other factors like increased potency likely play a key role.

Side Effects of Alprazolam
According to the FDA, the most likely side effects to stem from alprazolam usage include:
- Anxiety
- Confusion
- Constipation
- Depression/Suicidal ideations
- Dizziness
- Dry Mouth
- Extended pharmacological activity (e.g., drowsiness or light-headedness)
- Headache
- Insomnia
Rarer but more significant adverse effects include:
- Akathisia
- Blurred vision
- Dermatitis/Allergy
- Hypotension
- Rigidity
- Syncope
- Tachycardia
- Tremors
Alprazolam’s FDA label warns of the significant dangers of alprazolam dependence, withdrawal, and misuse. Additionally, the FDA takes great pains to ward users off concomitant opioid usage and stresses several contraindications to alprazolam, like pregnancy and use with heavy machinery.

Benzodiazepine Withdrawal & Dependence
Benzodiazepines are listed in the lowest category in terms of danger (Schedule IV), but their use should not be taken lightly. This drug class carries considerable risks even when used correctly and following a prescription.
Studies indicate that benzodiazepines, even when used for a short period, have a significant capacity to cause psychological and physical dependence. One study, for example, concluded that approximately one-third of individuals who use benzodiazepines for longer than four weeks experienced dependence and withdrawal symptoms after concluding their treatment [5].
Benzodiazepine withdrawal has been compared to alcohol and barbiturates, which shows just how serious it can be. Withdrawal fatalities are rare, but the generally accepted consensus is that they’re most common with alcohol, benzodiazepines, and opioids.
When it comes to alprazolam, there are certain things users should be aware of. Technically speaking, alprazolam has certain characteristics that make it less likely to cause dependence and withdrawal. It has a relatively quick elimination half-life and doesn’t produce metabolites that contribute significant pharmacological effects. However, it does have other attributes that can be dangerous like its high potency.
Independent of its individual aspects, the figures surrounding alprazolam misuse are significant and should concern anyone that’s considering taking the drug.

Harm Reduction: Alprazolam
- Don’t mix — Mixing benzodiazepines with other depressants (alcohol, GHB, phenibut, barbiturates, opiates) can be fatal.
- Take frequent breaks — Benzodiazepines can form dependence quickly, so it’s important to stop using the drug periodically.
- Know the dose — The dosage of benzos can vary substantially. Some drugs require 20 or 30 mg, others can be fatal in doses as low as 3 mg.
- Know who should NOT use benzos for any reason — Benzodiazepines are significantly more dangerous in older people or those with certain medical conditions.
- Test your drugs — If ordering benzos from unregistered vendors (online or street vendors), order a benzo test kit to ensure your pills contain what you think they do.
- Never snort or inject benzos — Not only does this provide no advantage, but it’s also extremely dangerous. Benzos should be taken orally.
- Recognize the signs of addiction — Early warning signs are feeling like you’re not “yourself” without the drug or hiding your habits from loved ones.
- Know where to go if you need help — Help is available for benzodiazepine addiction; you just have to ask for it. Look up “addiction hotline” for more information where you live. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
General Considerations
The most effective harm-reduction methods, especially when taking prescription drugs, are the common sense ones. Only use alprazolam if you have a legitimate doctor’s prescription and if so, make sure to follow instructions regarding dosage and other relevant factors.
In general, benzodiazepines are prescribed for the shortest time frame possible to limit the possibility of dependence and withdrawal symptoms, although this varies on a case-by-case basis. It’s always a good idea to keep this rule of thumb in mind: the more a drug is consumed, the more likely it will form a dependence.
Before seeking out a possible benzodiazepine prescription, you should familiarize yourself with the possible side effects and weigh those considerations against the reasons for using it. At the very least, consider a couple of non-pharmacological options. Behavior-related solutions like therapy or exercise and plant-based medical alternatives work wonders for some people.

Harmful Interactions
When dealing with benzodiazepines, there are a couple of drug interactions to avoid. Opioids and alcohol are a major concern, but be wary of other nervous system depressants. The FDA has issued several warnings stating that combining CNS depressants raises risk levels significantly. Mixing these drugs can put one at risk of respiratory depression — the leading cause of death in drug overdoses.
You should also know how alprazolam interacts with other compounds that affect CYP enzymes. These enzymes metabolize many medications. CYP inhibitors make the metabolization process less efficient, which can lead to an increased presence of alprazolam within the body and, thus, a higher risk of adverse effects. CYP inducers accelerate the metabolization process and, in turn, make alprazolam less effective.
Contraindications
There are several contraindications to alprazolam that users need to be aware of. For instance: alprazolam, and benzodiazepines in general, can raise the risk of congenital abnormalities during pregnancy. Another contraindication is the use of heavy machinery and driving. If a user’s job implies an activity of this sort, then taking alprazolam should be avoided.
Alprazolam Dosage
Proper dosage of benzodiazepines like alprazolam is one of the key factors in minimizing the risk. However, if a drug has multiple indications and several methods of administration, this can become slightly complicated.
According to the Mayo Clinic, alprazolam (oral route) has the following dosages for each indication and age group:
For Anxiety:
Oral dosage forms (solution, tablets, or orally disintegrating tablets):
| Age group | Dosage recommendations |
| 🧑🏻 Adults | At first, 0.25 to 0.5 milligrams (mg) 3 times a day. Your doctor may increase your dose as needed. However, the dose is usually not more than 4 mg per day. |
| 👨🏽🦳 Older adults | At first, 0.25 mg 2 or 3 times a day. Your doctor may increase your dose as needed. |
| 🧒🏼 Children | Your doctor must determine the use and dose. |
For Panic Disorder:
Oral dosage form (extended-release tablets):
| Age group | Dosage recommendations |
| 🧑🏻 Adults | At first, 0.5 to 1 milligram (mg) is taken daily in the morning. Your doctor may increase your dose as needed. However, the amount is usually not more than 10 mg per day. |
| 👨🏽🦳 Older adults | At first, 0.5 mg is taken in the morning once daily. Your doctor may increase your dose as needed. |
| 🧒🏼 Children | Your doctor must determine the use and dose. |

Similar Benzodiazepines
There are many benzodiazepines with effects that overlap with alprazolam, but only a few that are comparable in terms of the potency.
Here are some of the most closely-related benzodiazepines in terms of effects:
1. Clonazepam
Clonazepam and alprazolam are often mentioned together as they are the two high-potency benzodiazepines approved for treating panic disorder in the United States. Other high-potency benzodiazepines, such as bromazepam or lorazepam, aren’t frequently prescribed for this reason, while medium-potency benzodiazepines are not recognized as efficacious [6].
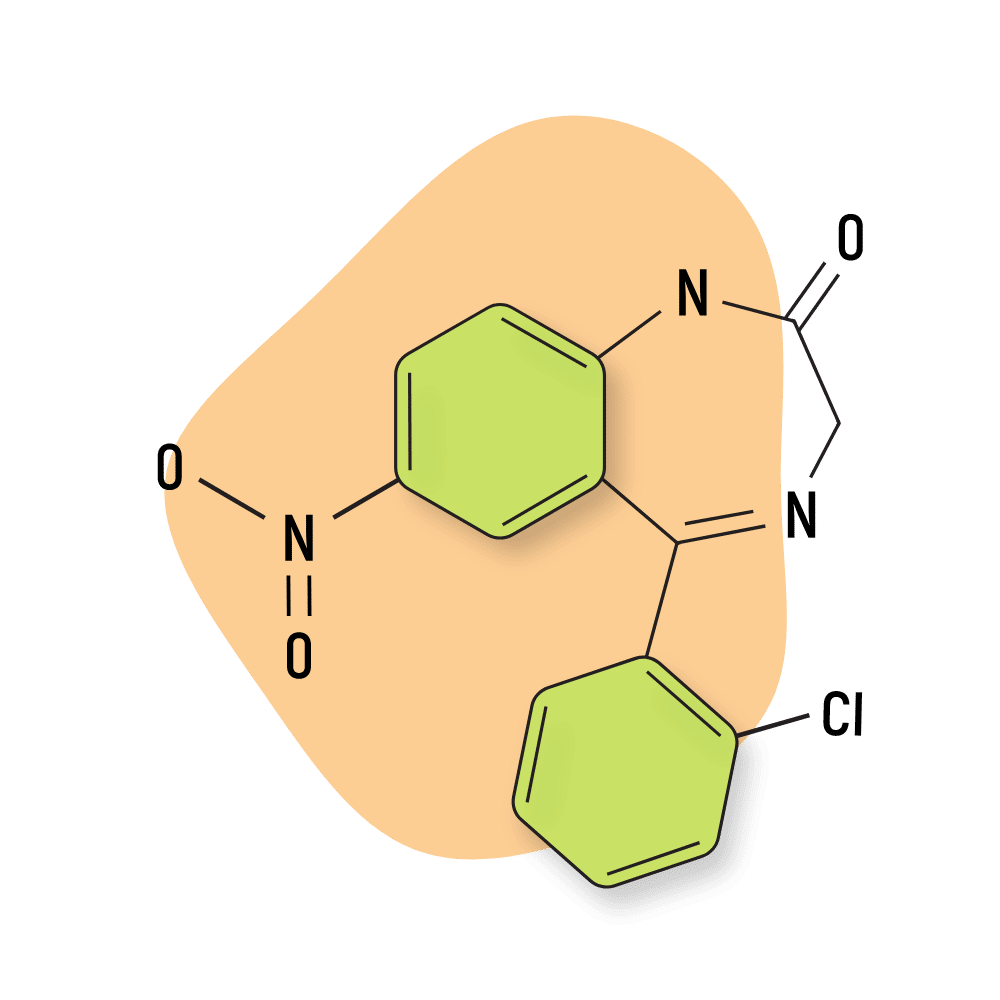
2. Lorazepam
Lorazepam — sold commercially as Ativan — has numerous similarities with alprazolam.
Both drugs have almost the same exact indications: management of anxiety disorders, short-term relief of anxiety symptoms, and short-term relief for depressive symptoms. The only difference in this sense is that alprazolam is approved for treating panic disorders, while lorazepam is not.
Both drugs also share substantial similarities in their pharmacokinetics and share an elimination half-life of around 12 hours. Lorazepam’s effects last for eight hours, while alprazolam lasts for five hours.
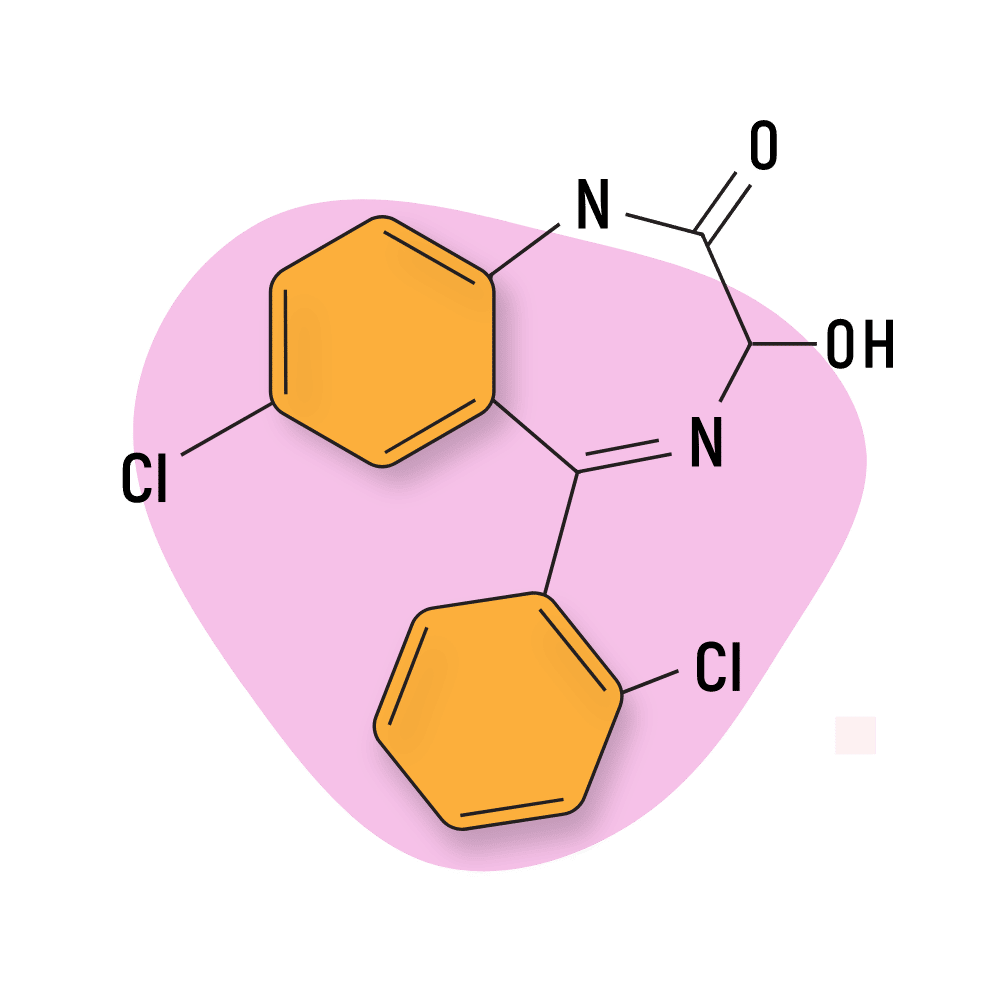
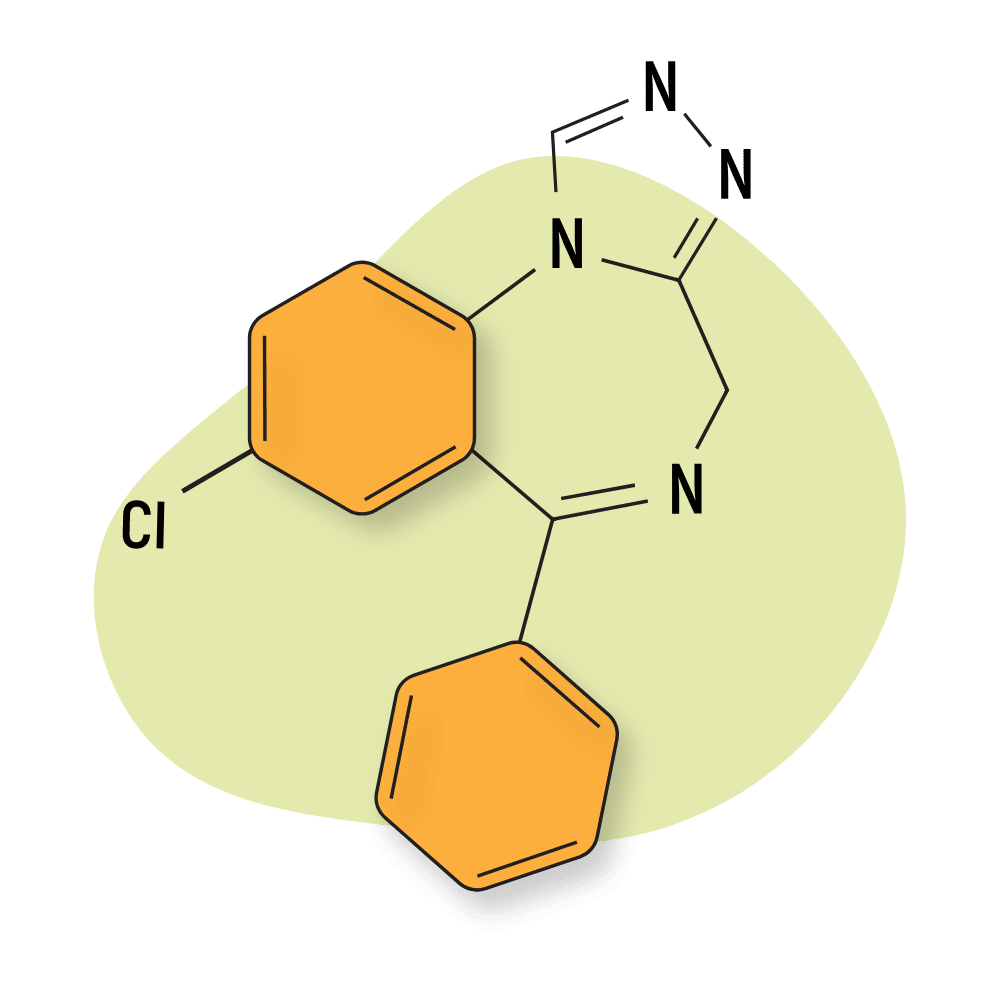
3. Triazolam
Like alprazolam, triazolam (Halcion) belongs to the triazolobenzodiazepine subtype. This suggests that they share a similar chemical structure, as well as certain pharmacological properties like high potency.
Triazolam is roughly twice as potent as alprazolam and has a stronger sedative action.
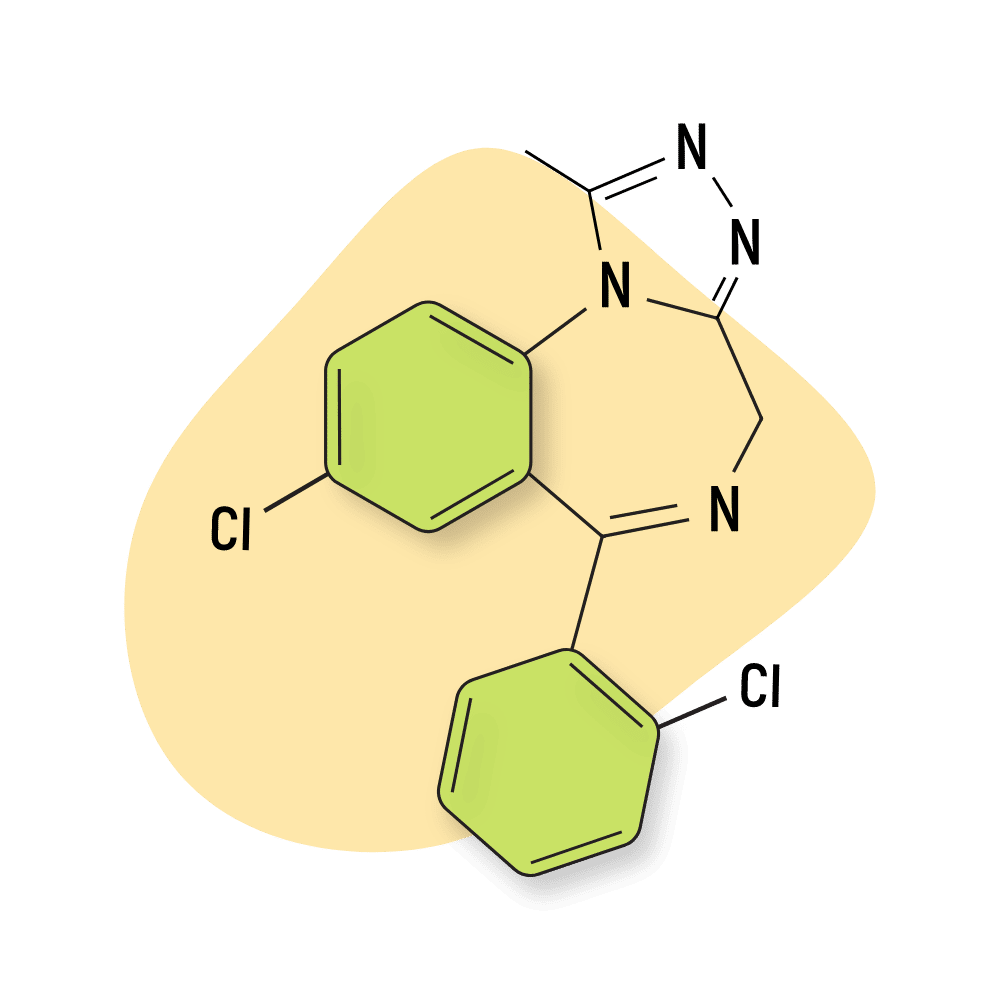
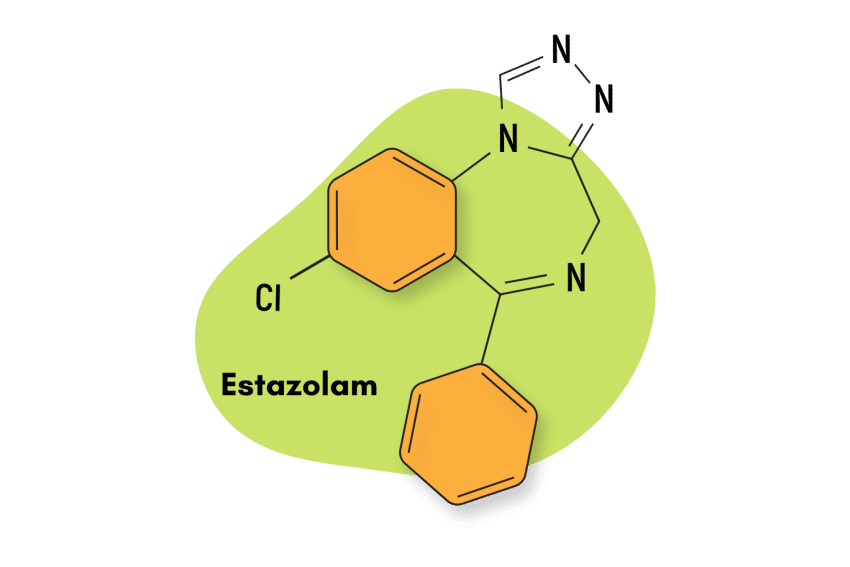
4. Estazolam
Estazolam is also a triazolobenzodiazepine and shares in the signature high-potency effects of this benzodiazepine subtype. However, unlike alprazolam, it is intermediate-acting and is only clinically approved for the treatment of sleep disorders.
Alternatives to Benzodiazepines
As more people become aware of the dangers involved in benzodiazepine usage, the interest in non-pharmacological treatment options for anxiety and depression-related disorders has begun to explode.
What’s more, with the surge in popularity of several natural anxiolytic compounds, there has never been a better time to consider a plant-based alternative.
The kava plant (Piper methysticum) should be a go-to for anyone looking to treat their anxiety with an all-natural remedy. Research has proved that the kava plant can induce states of calm and relaxation and is far safer than benzodiazepines — or any prescription product, for that matter [7].
Another solid option is the kratom plant (Mitragyna speciosa). Because it acts on the body’s opioid receptors, the kratom plant has received a lot of bad press, but — in reality — much of that is completely overblown. Kratom can be dangerous when combined with drugs and alcohol (especially other CNS depressants) but is very safe when used properly. The kratom plant has anxiolytic and relaxant properties when consumed in mid-to-high dose ranges [8].

Alprazolam FAQs
1. What formulations is alprazolam available in?
- Alprazolam (regular release) is available in orally disintegrating tablets of 0.25 mg, 0.5 mg, 1 mg, and 2 mg
- Alprazolam (extended-release) is available in orally disintegrating tablets of 0.5 mg, 1 mg, 2 mg, and 3 mg
- Liquid alprazolam is available in a 1 mg/mL oral concentrate
2. Does the presence of food affect the functioning of alprazolam?
Studies have shown that no significant changes in drug absorption occur when food is present. However, in a fasted condition, the drug absorption rate decreased, although not to a meaningful extent [9].
References
- Ait-Daoud, N., Hamby, A. S., Sharma, S., & Blevins, D. (2018). A review of alprazolam use, misuse, and withdrawal. Journal of addiction medicine, 12(1), 4.
- Campo, Soria, C., Chang, Y., & Weiss, D. S. (2006). Mechanism of action of benzodiazepines on GABAA receptors. British journal of pharmacology, 148(7), 984-990.
- Sieghart, W., & Sperk, G. (2002). Subunit composition, distribution and function of GABA-A receptor subtypes. Current topics in medicinal chemistry, 2(8), 795-816.
- Masiulis, S., Desai, R., Uchański, T., Serna Martin, I., Laverty, D., Karia, D., … & Aricescu, A. R. (2019). GABAA receptor signalling mechanisms revealed by structural pharmacology. Nature, 565(7740), 454-459.
- Riss, J., Cloyd, J., Gates, J., & Collins, S. (2008). Benzodiazepines in epilepsy: pharmacology and pharmacokinetics. Acta neurologica scandinavica, 118(2), 69-86.
- Chouinard, G. (2004). Issues in the clinical use of benzodiazepines: potency, withdrawal, and rebound. Journal of Clinical Psychiatry, 65, 7-12.
- Cairney, S., Clough, A. R., Maruff, P., Collie, A., Currie, B. J., & Currie, J. (2003). Saccade and cognitive function in chronic kava users. Neuropsychopharmacology, 28(2), 389-396.
- Swogger, M. T., & Walsh, Z. (2018). Kratom use and mental health: A systematic review. Drug and Alcohol Dependence, 183, 134-140.
- Erdman, K., Stypinski, D., Combs, M., Witt, P., Stiles, M., & Pollock, S. (2007). Absence of food effect on the extent of alprazolam absorption from an orally disintegrating tablet. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy, 27(8), 1120-1124.