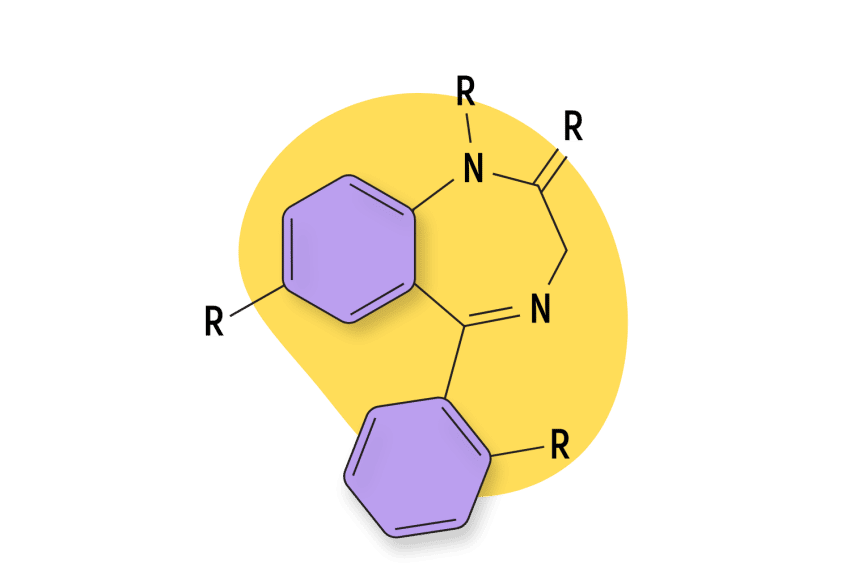
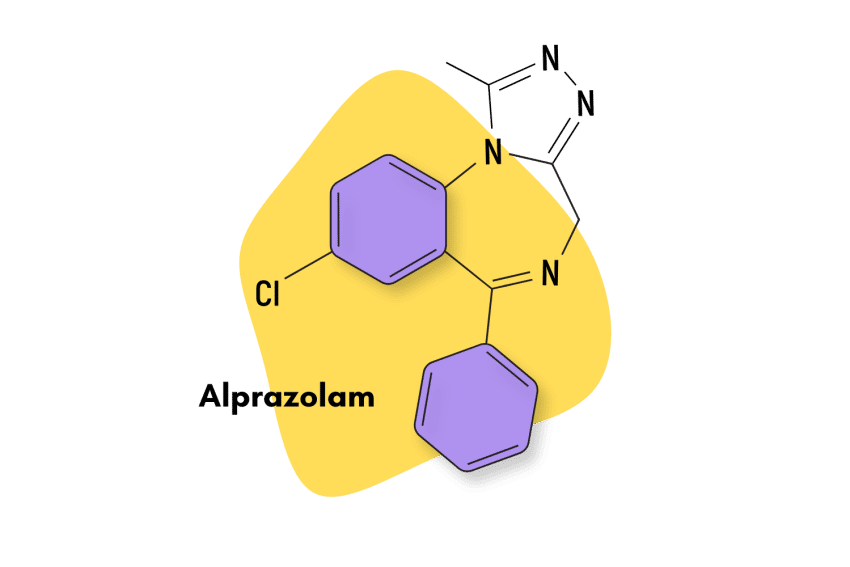
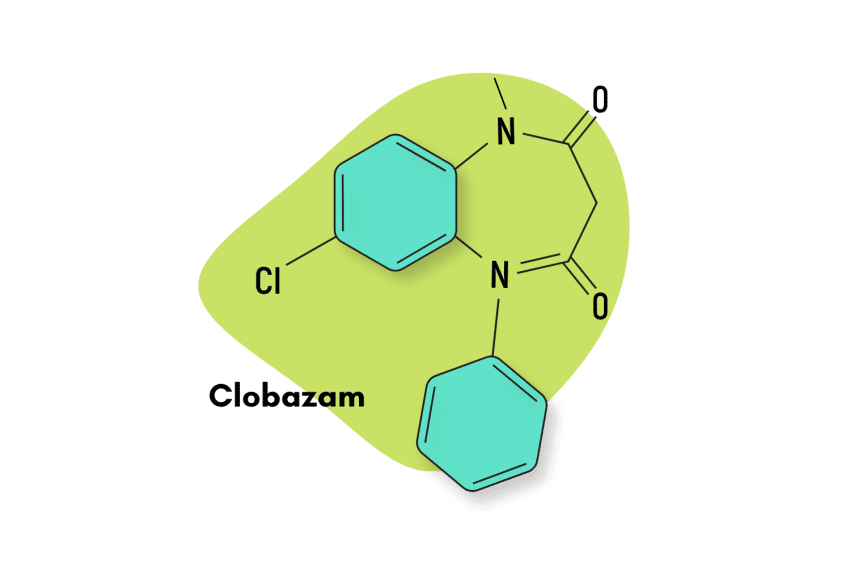
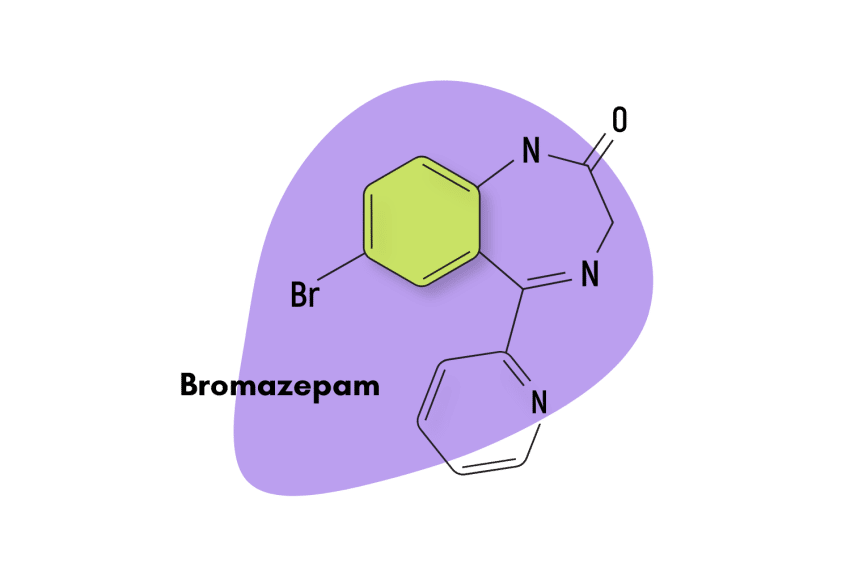
Oxazepam (Serax) Fact Sheet & Harm Reduction Guide
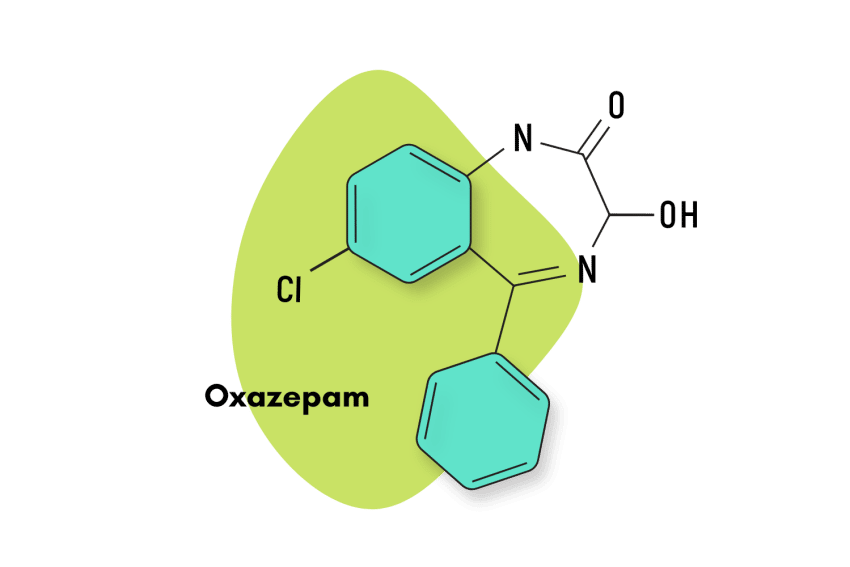
Oxazepam — sold under the brand names Serax and Alepam — is an intermediate-acting benzodiazepine (6–9 hour duration) used for treating anxiety, alcohol withdrawal symptoms, and more.
This benzo is weaker than other common benzodiazepines, such as alprazolam (Xanax) or clonazepam (Klonopin). It’s popular in some circles off-label for managing the side effects of stimulant drugs (not recommended).
Oxazepam shares the classical breadth of pharmacological functions normally found in all benzodiazepines but has only been clinically approved by the FDA for the treatment of anxiety-related disorders, as well as the symptoms of alcohol withdrawal.
However, oxazepam is also used for several off-label treatments (not approved by the FDA), including [1]:
- Catatonia
- Confusional arousals
- Insomnia
- Premenstrual dysphoric disorder
- PTSD
- Sleep continuation
- Sleep terrors
- Social phobia
Oxazepam Specs
| Status | Approved medication |
| Common Dosage | 10-30 mg |
| PubChem ID | 4616 |
| CAS# | 439-14-5 |
IUPAC Name: 7-chloro-3-hydroxy-5-phenyl-1,3-dihydro-1,4-benzodiazepin-2-one
Other Names: Serax, Alepam, Generics,
Metabolism: The metabolic clearance of oxazepam is not CYP mediated. It’s mainly polymorphically metabolized by glucuronide conjugation at the 3-carbon hydroxyl group, yielding stable diastereomeric glucuronides (R- and S-oxazepam glucuronide). It is excreted via the kidneys.
Duration of Effects: Oxazepam has an average elimination half-life of 8 hours. It does not produce any pharmacologically active metabolites.
Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Oxazepam Work?
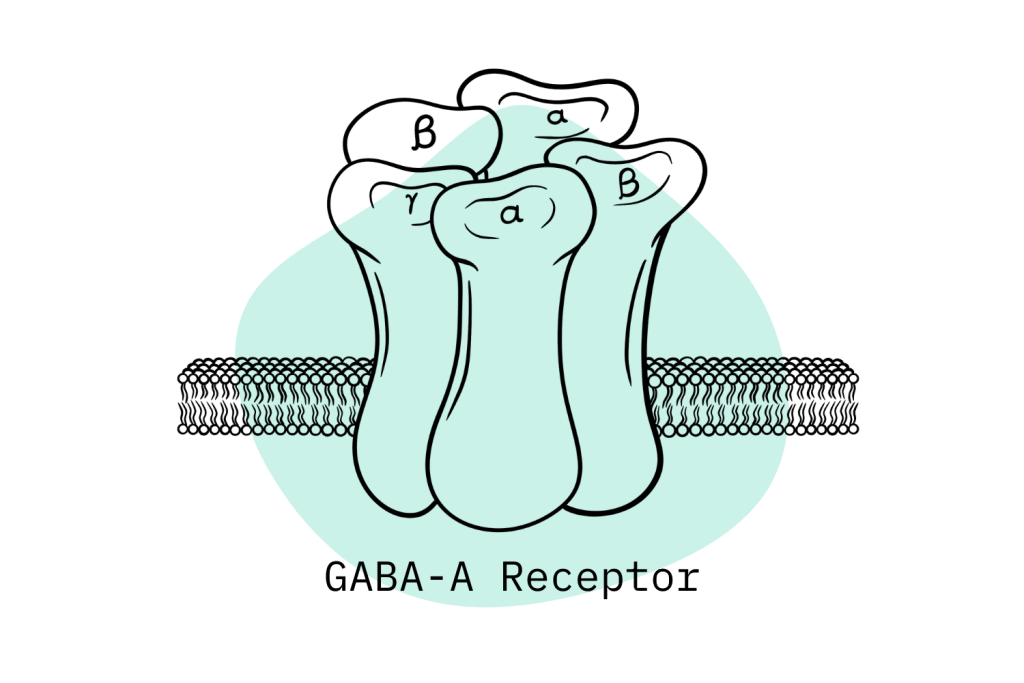
Oxazepam is a benzodiazepine of the 3-hydroxy family. It exerts its pharmacologic functions through the classic mechanism of action of most benzodiazepines: via the allosteric modulation of the GABA-A receptors in the brain and central nervous system (CNS) [2].
Gamma-aminobutyric acid, more commonly known as GABA neurotransmitters, is the chief inhibitory compound in the body. They’re responsible for the anxiolytic, hypnotic, and muscle relaxant properties associated with benzodiazepines.
Benzodiazepines work by increasing the natural inhibitory function of GABA-A neurotransmitters through what is known as an allosteric effect. This means benzodiazepines “boost” the effects of naturally occurring GABA rather than binding and activating the receptors themselves.
The inhibitory function of GABA means that neurons in the brain and CNS are far less likely to fire off an action potential: the electrical signals used by neurons. This, in turn, leads to an overall decrease in brain and CNS activity which is the primary cause of the pharmacological effects of benzodiazepines.
Oxazepam Specifics
We don’t know much about the specific functioning of the GABA-A molecule and how each individual benzodiazepine interacts with it to produce their slightly varying pharmacological profiles. However, for each benzodiazepine, we can usually identify a few factors that contribute to the overall profile in important ways.
In fact, researchers are increasingly attempting to identify the links between factors such as receptor binding affinity and pharmacokinetics [3].
When it comes to oxazepam, for instance, a British study has identified it as being one of the compounds with the slowest onset of action and the slowest rate of absorption out of all commercially available benzodiazepines [4].
These pharmacokinetic characteristics inevitably affect what situations oxazepam is clinically suited for. For example, because of its low absorption rate, oxazepam has great success when prescribed to individuals who have trouble staying asleep rather than falling asleep.
As an active metabolite of other classical benzodiazepines like diazepam, oxazepam’s metabolic characteristics are also relevant. Generally, it is a safer benzodiazepine because it does not utilize hepatic oxidation. Instead, oxazepam is cleared through the more simple process of glucuronidation.
Similarly to lorazepam, this means oxazepam is far less likely to accumulate in the body and cause adverse reactions in elderly patients or those with hepatic impairment: two common contraindications for high-potency benzodiazepines. Oxazepam does not form any active metabolites.
Is Oxazepam Safe? Risks & Side Effects
Like most other benzodiazepines, Oxazepam is listed in the Controlled Substances Act as a Schedule IV substance. This designation signifies that oxazepam is a compound with recognized medical benefits but still carries with it the potential for misuse and physical dependence. In recent years, however, the danger to public health posed by benzodiazepines is not quite in keeping with the Schedule IV classification of benzodiazepines.
Studies by public health organizations like the CDC and the National Institute on Drug Abuse (NIDA) have shown how a smaller but still significant benzodiazepine misuse situation has developed as a sort of adjunct crisis to the larger opioid epidemic. This situation largely reflects a rise in polydrug abuse in the United States and the pharmacological danger inherent in concomitant CNS depressant use.
For example, a 2020 CDC study has demonstrated how, in that year, benzodiazepines were involved in 12,290 deaths in the US.
A similar NIDA study allows us to further contextualize the role of benzodiazepines in this situation. The study concluded that in 2020, 16% of overdose deaths involving opioids also showed the presence of benzodiazepines.
There is undoubtedly a generalized danger when it comes to benzodiazepine misuse, but when it comes to the role of individual benzodiazepines, the situation can vary quite a lot. In the case of oxazepam, the specific pharmacological characteristics of the drug, such as its low potency, its slow rate of absorption, and the fact that it produces no active metabolites, means that its risk profile is actually more benign than that of most other benzodiazepines.

Side Effects of Oxazepam
According to the FDA, the necessity for discontinuing therapy with oxazepam due to side effects has been rare. Transient, mild drowsiness is commonly seen in the first few days of therapy. If it persists, the dosage should be reduced. In a few instances, dizziness, vertigo, headache, and syncope (rare) have occurred, either alone or with drowsiness.
Paradoxical reactions have been reported in some patients. These reactions may be secondary to relieving anxiety and usually appear in the first two weeks of therapy.
Other side effects identified during oxazepam therapy include:
- Altered libido
- Edema
- Lethargy
- Minor diffuse skin rashes (morbilliform, urticarial, and maculopapular)
- Nausea
- Slurred speech
- Tremors
These side effects are usually rare and are generally controlled with a dosage reduction.
Rare instances of leukopenia, hepatic dysfunction, and jaundice have also occurred. Lastly, ataxia has also been reported in rare instances and does not appear to be related to dosage.
Benzodiazepine Withdrawal & Dependence
In keeping with its Schedule IV classification, oxazepam use can cause physical dependence among users. Because of this, as a general rule, the sudden discontinuation of benzodiazepine therapy is not advised. Additionally, doctors usually attempt to prescribe benzodiazepines for the shortest time frame possible to limit the possibility of causing physical dependence.
Regarding benzodiazepines, withdrawal symptoms are more dangerous than other drug types and can even be fatal. This is because benzodiazepine tolerance, which entails both reduced GABA activity and increased glutamate activity, can lead to an inability of the neurological system to regulate hyperactive states. Excessive glutamate levels can also lead to a condition called excitotoxicity which, if left unchecked, can lead to neuronal damage, seizures, coma, and even death [6].

Harm Reduction: Oxazepam
With the explicit goal of reducing harm to all users, including those who engage in misuse, this section will attempt to lay out some common harm-reduction strategies that users can always refer to.
First, users who have not already begun benzodiazepine therapy should take the time to consider other alternatives available to them, as well as possible risk factors that could affect their therapy. For instance, a known history of drug or alcohol abuse has been shown to raise the possibility of prescription drug misuse. When it comes to benzodiazepines, that factor is quite dangerous. Users should take the time to carefully consider the benefits and drawbacks of benzodiazepine therapy.
It is also advisable for potential users to at least attempt a non-pharmacological solution to their problems before going ahead with benzodiazepine therapy. Behavior-related solutions like therapy or exercise are great options. If that doesn’t work, there are always plant-based medications like kava or kratom, which have similar properties to benzodiazepines while also having fewer side effects.
If a potential user decides to go ahead with benzodiazepine therapy, they should always keep certain rules of thumb that will help them stay safe. First, the two factors that most influence the formation of physical dependence are dosage quantity and the length of time of treatment. Basically, the longer benzodiazepine is used and the more they are used, the likelier it is for dependence to form.
And second: most instances of serious adverse effects and fatalities tend to be related in some way to misuse. Recreational misuse is an obvious thing to avoid, but there are other, subtler ways to misuse benzodiazepines. For instance, altering dosage quantities to treat a new ailment without your doctor’s knowledge would also be considered misuse.
Benzodiazepine Harm Reduction Tips
- 🥣 Don’t mix — Mixing benzodiazepines with other depressants (alcohol, GHB, phenibut, barbiturates, opiates) can be fatal.
- ⏳ Take frequent breaks or plan for a short treatment span — Benzodiazepines can form dependence quickly, so it’s important to stop using the drug periodically.
- 🥄 Always stick to the proper dose — The dosage of benzos can vary substantially. Some drugs require 20 or 30 mg; others can be fatal in doses as low as 3 mg.
- 💊 Be aware of contraindications — Benzodiazepines are significantly more dangerous in older people or those with certain medical conditions.
- 🧪 Test your drugs — If ordering benzos from unregistered vendors (online or street vendors), order a benzo test kit to ensure your pills contain what you think they do.
- 💉 Never snort or inject benzos — Not only does this provide no advantage, but it’s also extremely dangerous. Benzos should be taken orally.
- 🌧 Recognize the signs of addiction — Early warning signs are feeling like you’re not “yourself” without the drug or hiding your habits from loved ones.
- ⚖️ Understand the laws where you live — In most parts of the world, benzodiazepines are only considered legal if given a prescription by a medical doctor.
- 📞 Know where to go if you need help — Help is available for benzodiazepine addiction; you just have to ask for it. Look up “addiction hotline” for more information about where you live. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
Harmful Interactions to Avoid With Oxazepam
It is always important to watch out for harmful drug interactions when dealing with prescription drugs. In the case of benzodiazepines, users should always abstain from also using any other CNS depressant.
Mixing drugs that have a depressive effect on the CNS will put users in danger of respiratory depression: the leading cause of death in drug overdoses. This danger is present even if one of those CNS depressants is not a pharmacological compound. For instance, the kratom plant is a natural compound that is relatively safe. Still, because of its CNS depressant qualities, it is risky to try mixing it with a benzodiazepine.
If a prescription drug’s metabolism is CYP-mediated, users should also avoid other drugs that can potentially interfere with this process.
CYP enzymes are responsible for metabolizing a large percentage of pharmacological drugs, including some benzodiazepines. When other drugs are taken that can affect the CYP system, two things could happen:
- Metabolization could be inhibited or slowed — potentially leading to a drug buildup in the system.
- Metabolization could be increased — leading to rapid drug clearance and making treatment less effective.

Contraindications of Oxazepam
Pharmacological compounds often have a series of contraindications associated with them. Users must be aware of the contraindications of any compounds they are currently using as they might unknowingly be exposing themselves to risk in this way.
Contraindications are usually related to a series of special statuses, such as pregnancy, psychiatric conditions, hepatic impairment, etc. Certain esoteric drug combinations might also be contraindicated. This is why it’s so important for users to always check with a doctor when using a new pharmacological compound, even for recreational purposes.
The contraindications listed by the FDA for oxazepam include the following:
- History of hypersensitivity to benzodiazepines
- Myasthenia gravis
- Chronic obstructive pulmonary disease
- Severe hepatic disease
- Pregnancy
Oxazepam Dosage
According to the Mayo Clinic, these are the proper dosage quantities for oxazepam (oral solution):
For anxiety
| Age group | Dosage recommendations |
| 🧑🏻 Adults | 10 to 30 milligrams (mg) 3 or 4 times a day. |
| 👨🏽🦳 Older adults | At first, 10 mg 3 times a day. Your doctor may increase your dose if needed. |
| 🧑🏽🦱Children 6 years of age and older | Your doctor must determine the use and dose. |
| 🧒🏼 Children younger than six years of age | Use is not recommended. |
For alcohol withdrawal
| Age group | Dosage recommendations |
| 🧑🏻 Adults | 15 to 30 milligrams (mg) 3 or 4 times a day. |
Similar Benzodiazepines
As a classic 1,4- benzodiazepine, oxazepam shares many characteristics with other benzodiazepine compounds.
Diazepam
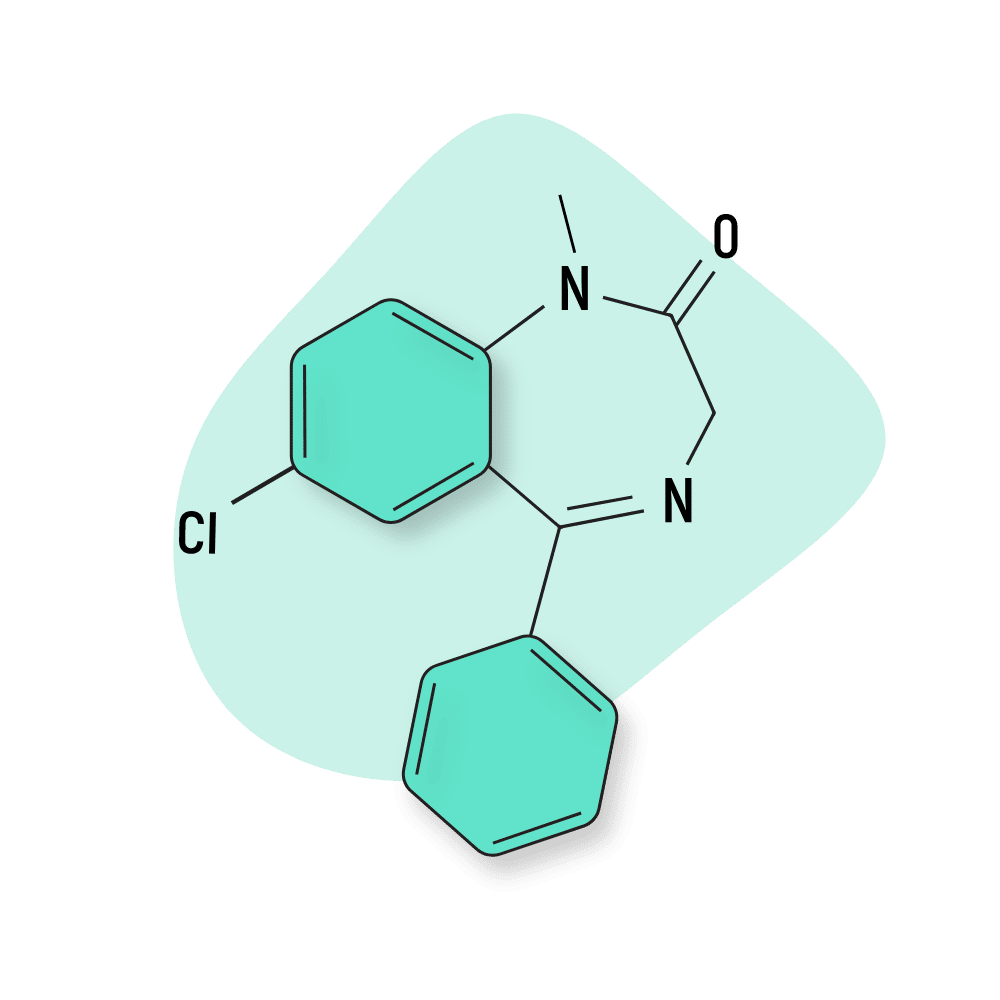
Oxazepam is a metabolic product of diazepam (Valium) and other known benzodiazepines, which means it holds specific pharmacological characteristics in common with its “father” compounds, like a comparable mechanism of action and a similar side effects profile, although oxazepam’s is more benign.
Lorazepam
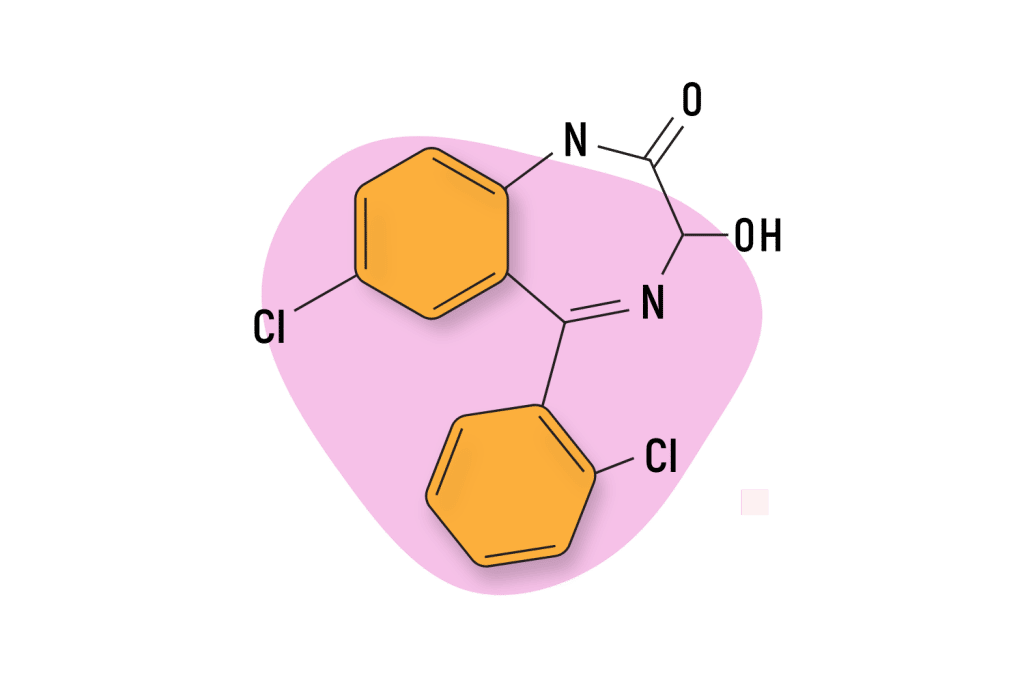
Lorazepam, another 1,4- benzodiazepine, shares many pharmacokinetic properties with oxazepam. Both oxazepam and lorazepam are intermediate-acting benzodiazepines with slow absorption rates and similar metabolic pathways, making them less prone to causing adverse effects.
Natural Alternatives to Benzodiazepines
Those looking for non-pharmacological alternatives to benzodiazepines are in luck. Plenty of natural compounds can achieve similar pharmacological benefits, all while posing fewer risks.
The kratom plant, for example, has gained a lot of popularity in recent years due to its amazing breadth of effects. When taken in low doses, it provides cognitive and euphoric benefits, while in mid-to-high doses, it can act as a pain killer and an anxiolytic (anti-anxiety) agent [7].
Another solid option is the valerian root, which contains several compounds that interact with GABA receptors similarly to benzodiazepines. Some of these compounds, like chatinine and valerianine, have the same allosteric effects on GABA-A receptors as benzodiazepines. However, users should be aware that the pharmacological potency of valerian root is less than that of benzodiazepines [8].

Oxazepam FAQs
What formulations are oxazepam available in?
Oxazepam is administered orally as a 10 mg, 15 mg, o4 30 mg capsule or as a 15 mg tablet. Dosing is without regard to meals.
What is the commercial situation of oxazepam today?
Oxazepam was popular during the 1960s as a treatment for anxiety, insomnia, and alcohol withdrawal. However, today it has been largely cast aside in favor of stronger, faster-acting, or longer-lasting drugs.
Does oxazepam have pharmacologically active byproducts?
As a metabolic byproduct of other approved medications such as diazepam, prazepam, and temazepam, oxazepam is a simple benzodiazepine and does not form any pharmacologically active byproducts.
References
- Alvan, G., & Odar-Cederlof, I. (1978). The pharmacokinetic profile of oxazepam. Acta Psychiatrica Scandinavica, 58(S274), 47-55.
- Guidotti, A., Baraldi, M., & Costa, E. (1979). 1, 4-Benzodiazepines and gamma-aminobutyric acid: pharmacological and biochemical correlates. Pharmacology, 19(5), 267-277.
- Vgontzas, A. N., Kales, A., & Bixler, E. O. (1995). Benzodiazepine side effects: role of pharmacokinetics and pharmacodynamics. Pharmacology, 51(4), 205-223.
- Serfaty, M., & Masterton, G. (1993). Fatal poisonings attributed to benzodiazepines in Britain during the 1980s. The British Journal of Psychiatry, 163(3), 386-393.
- Dinis-Oliveira, R. J. (2017). Metabolic profile of oxazepam and related benzodiazepines: clinical and forensic aspects. Drug metabolism reviews, 49(4), 451-463.
- Thornton, S. L., Whitacre, J., Pallo, N., Roberts, N., & Oller, L. (2021). A Retrospective Review of Morbidity and Mortality Associated with Acute Benzodiazepine Withdrawal at a Midwestern Academic Medical Center. Kansas Journal of Medicine, 14, 77.
- Swogger, M. T., & Walsh, Z. (2018). Kratom use and mental health: A systematic review. Drug and Alcohol Dependence, 183, 134-140.
- Patočka, J., & Jakl, J. (2010). Biomedically relevant chemical constituents of Valeriana officinalis. Journal of applied biomedicine, 8(1), 11-18.