Benzodiazepine Use: A Look at Who’s Using Them & What the Numbers Mean
The global movement towards the destigmatization of mental health, coupled with growing concerns around the overprescription of psychiatric drugs, has led to an increased interest in using certain drugs like benzodiazepines. This article will examine the available data to examine recent trends in benzodiazepine use.
What Are Benzodiazepines?
Once the most widely prescribed medication, benzodiazepines — also known as “benzos”— are an important class of psychoactive drugs. Chemically, benzodiazepines are depressants, which means they work to lower brain activity. They do this by being strong activators of the GABA neurotransmitter. GABA can block specific signals in your central nervous system and thus produce a calming effect.
This calming effect gives benzodiazepines their sedative, hypnotic (sleep-inducing), anxiolytic (anti-anxiety), anticonvulsant, and muscle relaxant properties. The medical uses of benzodiazepines are tied to these functions, and they’re used to treat conditions like insomnia, depression, seizures, anxiety-related disorders, and more.

Benzodiazepine Use Statistics
At a global level, benzodiazepine use is fairly widespread, but not like other drugs. A 2017 study by the Global Drug Survey found that 5.7% of respondents had used benzodiazepines within the past year. Such a rate is lower than that of alcohol (94.6%), tobacco (47.9), cannabis (46.3%), MDMA (21.7%), and cocaine (17.2%), but it is still significant.
When it comes to the U.S., though, benzodiazepine use has become more popular. Data from the 2015 to 2016 National Institute on Drug Abuse found that approximately 12.5% of adults in the United States use benzodiazepines, which equates to roughly 30.5 million people.
Research is hard to find on why people take benzodiazepines, but one study points to anxiety management and recreational use as the biggest reasons [6].
Benzodiazepine Prescriptions
Another study has shed light on how benzodiazepines are prescribed to the general public [7]. The study examined 386,457 ambulatory care visits from 2003 to 2015 and found several interesting data points.
The rise in benzodiazepine prescriptions seems driven mainly by primary care physicians. In 2003, they had been prescribing the drug at a rate of 3.6%. This figure jumped to 7.5% in 2015 [2]. The increase is notable because when we look at psychiatrists, for example, the rate only increased from 29.6% to 30.2%. It was also found that benzodiazepines are commonly prescribed with other medications used for sedation.
According to the figures, the most popular benzodiazepines, by estimated prescription numbers, are:
- Alprazolam: 17,533,262
- Clonazepam: 15,578,495
- Lorazepam: 10,875,212
- Diazepam: 5,711,206
Who is Using Benzodiazepines?
There are two main groups of benzodiazepine users — those that take it as a prescription for insomnia, anxiety, or injuries involving the muscles; and those who take it recreationally as an inebriant or to offset side effects from other recreational drugs.
There are also several distinct patterns of use in people who take benzodiazepine drugs based on age, ethnicity, and gender.
Gender & Age Differences
The gender differences in benzodiazepine use are considerable: benzodiazepine use is nearly twice as prevalent in women as men [3].
Statistics show benzodiazepine use constantly rises with age:
College Students
There is also some data to consider when it comes to unprescribed use. A recent study by Healthy Minds Network found that benzodiazepine use is not uncommon for college students in the United States.
The most popular drug by far was marijuana, with 20% of respondents confirming they had used it in the past 30 days. Then, tied at 1% of respondents are stimulants like Adderal and Ritalin, benzodiazepines, and cocaine.
One might think that 1% isn’t huge, but it is surprising that benzodiazepines have the same rate of use in college students as stimulants and cocaine. Widespread knowledge about drug misuse gives the impression that the former drugs are much more popular.
Demographics
Unfortunately, there isn’t much data available regarding race differences and benzodiazepine use, but some general conclusions can be reached from the available information. Non-Hispanic Whites are more likely than non-Hispanic Blacks, Hispanics, and Asians to both use benzodiazepines and have a dependence [4].

Benzodiazepine Abuse Statistics
Most benzodiazepines are classified as Schedule IV drugs, which implies they have a lower potential for abuse and danger than those classified as schedule III. Still, they are recognized as having the potential to cause physical and mental dependence.
The general thinking around benzodiazepines is that, when taken properly, they are relatively safe, but they are still more dangerous than their Schedule IV classification makes them seem. When taken in combination with other drugs, especially opioids and alcohol, they can be quite deadly.
For instance, recent research has shown that 75% of benzodiazepine deaths also involve opioid usage [1]. In fact, it seems that in terms of prescription drug types, benzodiazepines and opioids are the two most dangerous types of drugs. According to the CDC, benzodiazepines were involved in 30% of drug overdose deaths in the United States in 2013, second only to opioids, which were involved in 70%.
In recent years, we have seen a worrying increase in drug overdose deaths, and benzodiazepines have a part to play there.
The following graph by the CDC shows the increase in overdose deaths involving benzodiazepines:
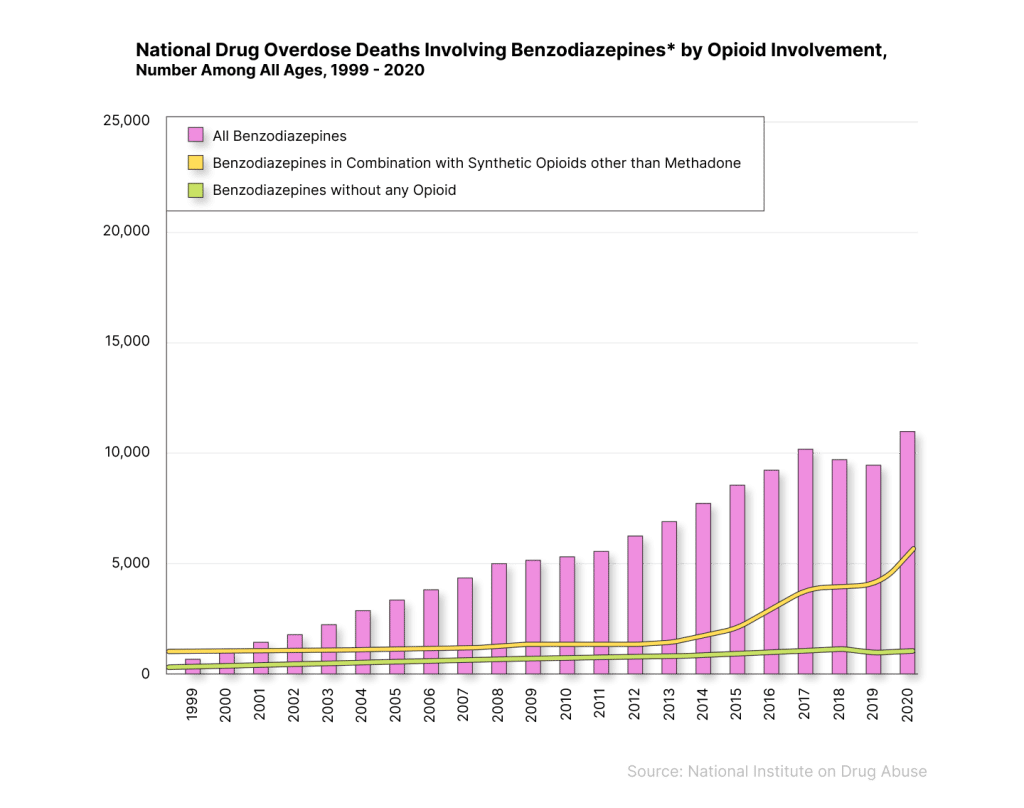
As we can see, benzodiazepine-related deaths have increased considerably since 1999, from 1,135 to 11,537. Between 2017 and 2020, deaths declined and rose again to 12,290. However, the yellow line shows much of the recent increase in fatalities was in combination with opioids.
It should be noted that benzodiazepine prescriptions also increased during this time. From 1996 to 2013, the latest date for this statistic, benzodiazepine prescriptions grew from 8.1 million to 13.5 million per year.
According to the National Institute on Drug Abuse, around 2.1% of users engage in misuse. However, only about 0.2% of them meet the requirements of a benzodiazepine use disorder.
When it came to misuse, the NIDA report found that the most prominent reasons were to improve sleep, reduce tension, or cope with stress. However, recreational use and dependence also played a part. Only 20% of users who engaged in misuse got the benzodiazepines from their doctor, indicating they did not have a prescription.
Benzodiazepine Withdrawal Statistics
Research is lacking on this question, but according to one study, 10-25% of chronic benzodiazepine users suffer from protracted withdrawal symptoms upon cessation of benzodiazepine use [8]. Both psychological and physical symptoms are common.

How Do Benzos Work?
Benzodiazepines work by activating the gamma amino butyric acid (GABA) neurotransmitter. GABA is responsible for breathing, memory, reasoning, emotions, and other essential functions. Benzos reduce this brain activity by blocking specific signals from going off in the central nervous system.
What Are the Risks of Using Benzos?
Common side effects among all benzodiazepine drugs include [5]:
- Blurry vision
- Dizziness
- Drowsiness
- Euphoria
- Fatigue
- Impaired motor coordination
- Lethargy
- Mood swings
- Slurred speech
- Vertigo
Possible Interactions
Drug interactions are common when dealing with benzodiazepines. Since they are metabolized in the liver via the cytochrome p450 system, drugs that either potentiate or attenuate cytochrome p450 enzymes will increase or decrease the elimination half-life of benzodiazepines [5].
As we have already seen, the potential for abuse with benzodiazepines is relatively high. According to the NIH, misuse accounts for 17.2% of all benzodiazepine use in the United States [8]. This misuse is highest in the 18-25 age group (5.2%), while adults over 65 had the lowest abuse (0.6%).
Comorbidities
Avoid benzodiazepines if you suffer from any of the following:
- Breathing problems
- Severe liver or kidney disease
- Severe lung disease
- Sleep apnoea
- Uncontrolled or severe myasthenia gravis
Be cautious with benzo use if you suffer from the following:
- Chest and lung problems
- Diagnoses personality disorder
- Liver problems
- Muscle weakness
- Porphyria

Conclusion: Benzo Use & Abuse
A clear picture of the situation is essential in determining whether there is a need to intervene in benzodiazepine use among the U.S. population. And from the available data, a general conclusion can be reached that, during recent years, benzodiazepine misuse has risen considerably in the United States.
It remains true that opioids are certainly more dangerous and carry a much larger responsibility when it comes to the increase in drug overdose deaths in the U.S. However, the problem of benzodiazepines, while still very serious, has somewhat failed to receive the level of attention it is due.
References
- Jones, C. M., & McAninch, J. K. (2015). Emergency department visits and overdose deaths from the combined use of opioids and benzodiazepines. American journal of preventive medicine, 49(4), 493-501.
- Agarwal, S. D., & Landon, B. E. (2019). Patterns in outpatient benzodiazepine prescribing in the United States. JAMA network open, 2(1), e187399-e187399.
- Olfson, M., King, M., & Schoenbaum, M. (2015). Benzodiazepine use in the United States. JAMA psychiatry, 72(2), 136-142.
- Cook, B., Creedon, T., Wang, Y., Lu, C., Carson, N., Jules, P., … & Alegría, M. (2018). Examining racial/ethnic differences in patterns of benzodiazepine prescription and misuse. Drug and alcohol dependence, 187, 29-34.
- Griffin, C. E., Kaye, A. M., Bueno, F. R., & Kaye, A. D. (2013). Benzodiazepine pharmacology and central nervous system–mediated effects. Ochsner Journal, 13(2), 214-223.
- Stein, M. D., Kanabar, M., Anderson, B. J., Lembke, A., & Bailey, G. L. (2016). Reasons for benzodiazepine use among persons seeking opioid detoxification. Journal of substance abuse treatment, 68, 57-61.
- Marra, E. M., Mazer‐Amirshahi, M., Brooks, G., Van Den Anker, J., May, L., & Pines, J. M. (2015). Benzodiazepine prescribing in older adults in U.S. ambulatory clinics and emergency departments (2001–10). Journal of the American Geriatrics Society, 63(10), 2074-2081.
- Maust, D. T., Lin, L. A., & Blow, F. C. (2019). Benzodiazepine use and misuse among adults in the United States. Psychiatric services, 70(2), 97-106.