Halazepam (Paxipam) Fact Sheet & Harm Reduction Guide
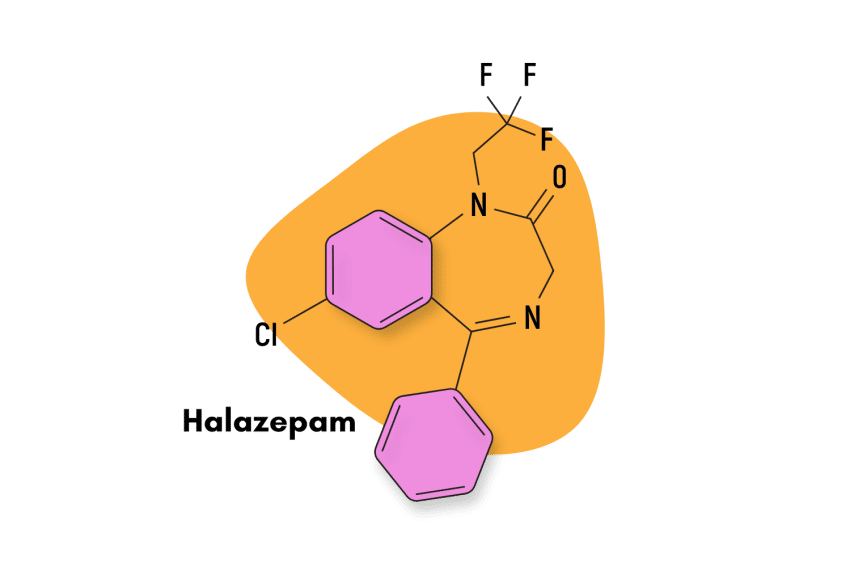
Halazepam is sold under the trade names Paxipam, Alapryl and Pacinone. It’s a benzodiazepine derivative belonging to the “classical” 1,4-benzodiazepine subtype.
Halazepam was created to market it as a “less toxic” diazepam. Structurally and pharmacologically, both compounds are incredibly similar. Both drugs produce the same effects, the only significant difference being that halazepam has a shorter duration of action [1].
Given its similarity with diazepam, both compounds are indicated for the same clinical objectives: the symptomatic relief of anxiety and tension associated with anxiety disorders or transient emotional disorders, as well as adjuvant treatment in pathological states in which anxiety, tension, and apprehension have been demonstrated.
In this sense, halazepam can best be considered an intermediate-acting benzodiazepine anxiolytic of average potency with some anticonvulsant potential.
Halazepam, however, is no longer marketed in the United States. The drug exhibited disappointing commercial results and was withdrawn by its manufacturer, Schering, in 2009.
Halazepam Specs
| Status | Approved medication (discontinued) |
| Common Dosage | 20-40 mg |
| PubChem ID | 31640 |
| CAS# | 23092-17-3 |
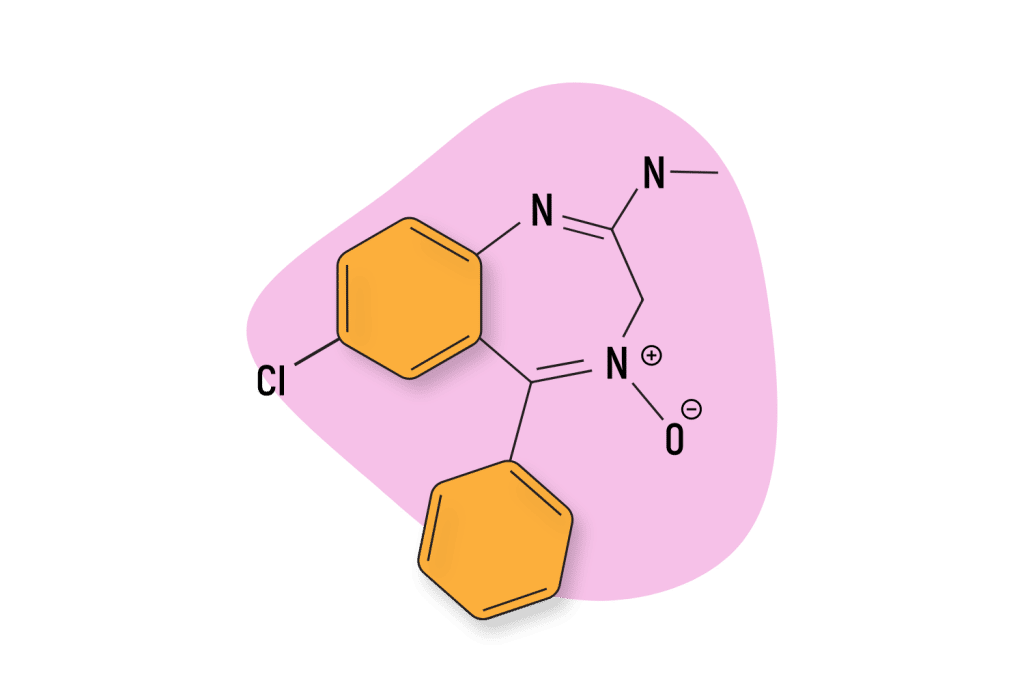
IUPAC Name: 7-chloro-5-phenyl-1-(2,2,2-trifluoroethyl)-3H-1,4-benzodiazepine-2-one
Other Names: Paxipam, Alapryl, Pacinone
Metabolism: the metabolic pathway of halazepam is hepatic. It’s dealkylated in the liver to the active compound N-desmethyldiazepam (nordiazepam), a significantly active metabolite with a long elimination half-life, which also has further active metabolites like oxazepam [2].
Duration of Effects: halazepam has an elimination half-life of 8 to 14 hours. However, if you include halazepam’s pharmacologically active metabolites in the equation, the total time for complete hepatic clearance can be as long as 200 hours.
Benzodiazepine Dosage Equivalency Calculator
**Caution:** Benzodiazepines have a narrow therapeutic window. Dose equivalents may not be accurate in higher doses.
This calculator does not substitute for clinical experience and is meant to serve only as a reference for determining oral benzodiazepine equivalence.
Please consult a medical practitioner before taking benzodiazepines.
How Does Halazepam Work?
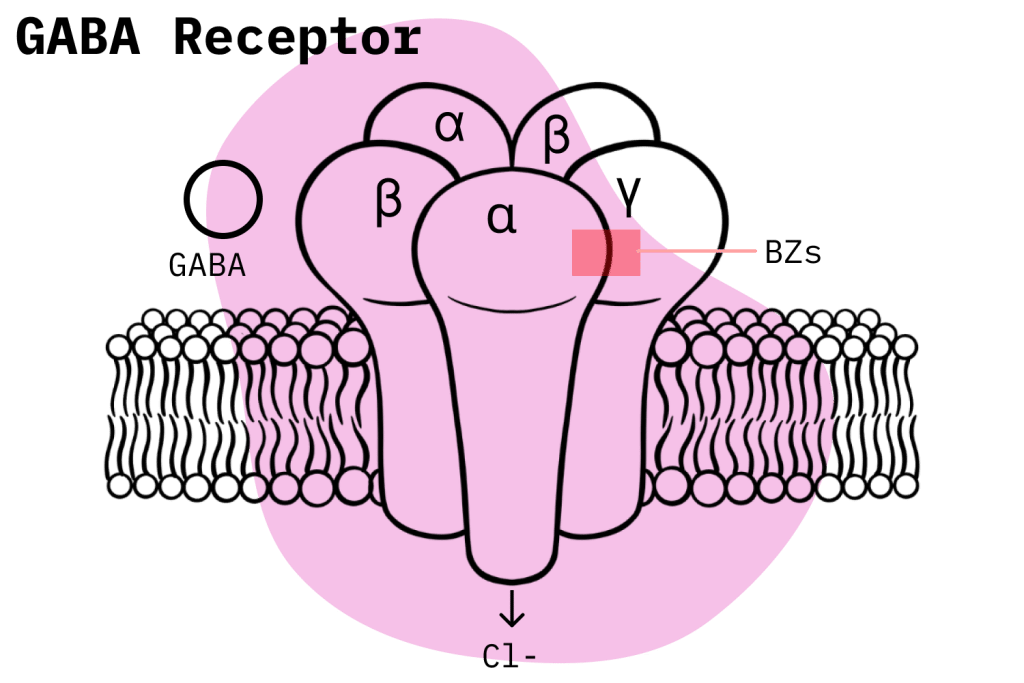
As a close analog to diazepam and chlordiazepoxide, halazepam also employs the standard GABA-mediated mechanism of action used by most benzodiazepines.
GABA, also known as gamma-aminobutyric acid, is the body’s primary inhibitory neurotransmitter. Benzodiazepines work through their interactions with GABA. Once benzodiazepines enter the body and bind to their given receptor sites on GABA-A receptors, they work to potentiate the natural inhibitory function of GABA through an allosteric effect. It’s important to note that while many compounds interact with GABA to produce effects comparable to benzodiazepines, that doesn’t mean they utilize the same GABA pathway.
Generally speaking, benzodiazepines achieve this effect by increasing the frequency of the chloride channel in GABA neurotransmitters. This results in a hyperpolarized cell membrane which prevents further cell excitation, leading to the generalized inhibition of the brain and central nervous system responsible for the associated benzodiazepine-like effects.
Studies have also shown that diazepam employs certain secondary pathways that contribute to its effect profile. Since halazepam is almost the same compound, both substances likely share similar characteristics.
Diazepam binds to the sodium channels, which might also contribute to its anticonvulsant properties [3]. It also has an affinity for a unique benzodiazepine receptor located on the mitochondrial membrane known as the “translocator protein (18 kDa) [4].
However, studies have also shown meaningful differences between diazepam and halazepam. Halazepam appears equal to or more effective than diazepam, with a lower frequency of side effects in treating both situational and characterologic anxiety [5].
Is Halazepam Safe? Risks & Side Effects
Nearly all prescription drugs carry a certain level of risk, which is why it’s always so important to know the risk level of the drug you’re using and what you can do to stay safe.
Regarding benzodiazepines, nearly all of these compounds share the same classification under the Controlled Substances Act, that being Schedule IV. Such a designation implies that a compound has recognized medical uses but also the potential to cause physical dependence and the associated withdrawal symptoms, albeit to a lesser degree than Schedule III compounds.
However, since all benzodiazepines share this designation, it’s hardly of any use if one wants to suss out the individual risk level of a given benzodiazepine. Furthermore, it’s no secret that agencies like the FDA and the DEA are not wholly objective entities. For instance, does it make sense that a substance like cannabis —which has proven medical benefits and no potential to cause fatalities —is still classified under Schedule I while opioid medications are listed under Schedule III & II?
For these reasons, it’s important for current and potential benzodiazepine users to do a little research or at least speak to a doctor about the particularities of whatever benzodiazepine they are considering.
In the case of halazepam, we can likely assume that it has a similar risk profile to diazepam, although studies have found that it is less toxic and produces fewer side effects. However, one characteristic that should be accounted for in terms of risk is the long elimination half-life of halazepam and its metabolites.
The primary metabolite of halazepam, N-desmethyldiazepam (nordiazepam), which also has metabolites of its own, can take as long as 200 hours to be cleared from the body. This implies certain risks, mainly the accumulation of halazepam within the body. The accumulation of a compound within the body can lead to an increased rate of side effects and can contribute to the formation of physical dependence. However, it also means the compounds present fewer chances of acute withdrawal symptoms and don’t promote drug addiction habits like compounds with a short duration of effects do.
Side Effects of Halazepam
Below are the side effects that studies have identified with the use of halazepam [5].
A) Very frequent (>25%): drowsiness, confusion, and ataxia, especially in the elderly and debilitated; if these symptoms persist, the dose should be reduced.
B) Frequent (10-25%): dizziness, sedation, headache, depression, disorientation, dysphasia or dysarthria, decreased concentration, tremor, changes in libido, urinary incontinence, urinary retention, nausea, vomiting, diarrhea, constipation, dryness mouth, hypersalivation, epigastric pain.
C) Occasional (1-9%): hepatitis, jaundice, dermatitis, urticaria, pruritus, leukopenia, agranulocytosis, anemia, thrombocytopenia, eosinophilia, behavioral disturbances, anterograde amnesia, paradoxical excitation, psychosis, vision disturbances, diplopia, nystagmus, hearing disturbances.
D) Rare (<1%): respiratory depression, hypotension, hypertension, bradycardia, tachycardia, palpitations
Additionally, it has been found that halazepam has a significant effect on electroencephalogram (EEG) tests. These are conducted in order to measure electrical activity in the brain. Furthermore, a marked difference in comparison with chlordiazepoxide and diazepam was that halazepam did not increase hostility or aggression in patients, as the former compounds are known to do.

Benzodiazepine Withdrawal & Dependence
Benzodiazepine users, both recreational and prescription, must always be on the lookout for the possible development of symptoms of physical dependence and withdrawal. Besides relatively minor side effects like headaches, nausea, drowsiness, and the like, the most latent adverse effect that benzodiazepine users worry about is the possibility of dependence.
This is true for many reasons. First, withdrawal symptoms stemming from benzodiazepines are more dangerous than one might think. In fact, along with those of alcohol, benzodiazepine withdrawals can be fatal. There are a couple of reasons for this. The use of benzos implies reduced GABA activity and increased glutamate activity, and when benzodiazepine use is ceased, this can result in a failure of regulation for hyperactive states. GABA and glutamate affectation can also lead to excitotoxicity, which can cause severe neuronal damage, leading to seizures, coma, or death.
Deaths stemming from benzodiazepine withdrawal are rare, but the fact that they can happen should show how serious a benzodiazepine dependence is.
A benzodiazepine dependence also implies the need for patients to engage in the process of drug tapering so they can safely get off benzodiazepines. This is something that doctors usually do anyways, as sudden cessation of benzodiazepine use is not recommended. Still, once the patient has developed withdrawal symptoms, the process is bound to be longer.

Harm Reduction: Halazepam
Harm reduction approaches to drug use are steadily gaining ground worldwide. Slowly but surely, governments realize that drug dependence cannot be treated punitively, as these approaches only worsen the problem. However, there are still many places where harm reduction knowledge is not freely distributed, so we want to lay out some basic recommendations in this section.
The main goal of staying safe with benzos is avoiding misuse. Only take as much as you need, avoid taking it for longer than two weeks, and never use them recreationally or off-label.
However, users should know that avoiding misuse is not enough to protect themselves from the possibility of benzodiazepine dependence. For this, it’s necessary to be a bit more proactive regarding your treatment. The most effective approach is to try and limit the following two factors by as much as possible: dosage (the total amount of benzodiazepines consumed) and duration (how much time you’re taking benzos on a day-to-day basis).
Before starting treatment, prescription users should talk to their doctor about limiting these factors.
In the case of recreational users, the harm reduction approach has to be a lot more practical. Here we are likely dealing with people with at least some history of drug abuse, and the main goal is to have them stay alive, not have them complete their benzo treatments without developing dependences.
The best recommendation in this regard is to never mix pharmacological compounds, whether prescription or not. However, if a user is deadset on mixing compounds, they should at least try to pick ones of lower potency and mix them little by little, not all at once.
Benzodiazepine Harm Reduction Tips:
- 🥣 Don’t mix — Mixing benzodiazepines with other depressants (alcohol, GHB, phenibut, barbiturates, opiates) can be fatal.
- ⏳ Take frequent breaks or plan for a short treatment span — Benzodiazepines can form dependence quickly, so it’s important to stop using the drug periodically.
- 🥄 Always stick to the proper dose — The dosage of benzos can vary substantially. Some drugs require 20 or 30 mg; others can be fatal in doses as low as 3 mg.
- 💊 Be aware of contraindications — Benzodiazepines are significantly more dangerous in older people or those with certain medical conditions.
- 🧪 Test your drugs — If ordering benzos from unregistered vendors (online or street vendors), order a benzo test kit to ensure your pills contain what you think they do.
- 💉 Never snort or inject benzos — Not only does this provide no advantage, but it’s also extremely dangerous. Benzos should be taken orally.
- 🌧 Recognize the signs of addiction — Early warning signs are feeling like you’re not “yourself” without the drug or hiding your habits from loved ones.
- ⚖️ Understand the laws where you live — In most parts of the world, benzodiazepines are only considered legal if given a prescription by a medical doctor.
- 📞 Know where to go if you need help — Help is available for benzodiazepine addiction; you just have to ask for it. Look up “addiction hotline” for more information about where you live. (USA: 1-800-662-4357; Canada: 1-866-585-0445; UK: 0300-999-1212).
Halazepam Drug Interactions
Like virtually all benzodiazepines, halazepam exerts its effects through a generalized depressive effect on the brain and central nervous system. As such, it should never be mixed with another compound with this property, as the effect can commonly lead to severe respiratory depression: the leading cause of death in drug overdoses.
This effect is so deadly that the concomitant use of opioids and benzodiazepines has led to an explosion in drug-related fatalities in the United States.
Users should also ask their doctors about the possibility of CYP drug interactions, which can affect the proper metabolic clearance of their given benzodiazepine.

Halazepam Contraindications
Halazepam is contraindicated for the following:
- Bronchitis
- Chronic obstructive pulmonary disease (COPD)
- Conjunctive use of barbiturates, opiates, or those suffering from alcoholism
- Intellectual disabilities due to frequent paradoxical reactions
- Major depression
- Myasthenia gravis
- Over the age of 65 (high risk)
- Personality disorders
- Sleep apnea
Halazepam Dosage
👩🏻 Adults: The optimal dose of halazepam should be individualized based on the severity of symptoms and the patient’s response. After several days of treatment, the patient’s response will allow the doctor to increase or decrease the dose. The recommended halazepam dose is 20 mg (half a 40 mg tablet) up to 40 mg three or four times daily. The total dose can vary between 80 to 160 mg daily. Halazepam can also be given as a single dose at bedtime.
👨🏽🦳 Elderly: In debilitated patients or the elderly over 70, the recommended initial dosage is 20 mg (half a 40 mg tablet) once or twice daily. The dose should be adjusted according to need and tolerance. The duration of treatment should be as short as possible. The patient should be reassessed regularly, including the need to continue treatment, especially in symptom-free patients. In general, the total duration of treatment should not exceed 8-12 weeks, including its gradual withdrawal. In some instances, it may be necessary to prolong the treatment beyond the recommended period; this decision can only be adopted by the doctor in charge of the patient after weighing the evolution of the patient.

Similar Benzodiazepines
There are two obvious benzodiazepine candidates with a high degree of similarity to halazepam.
Diazepam
Halazepam is an analog to diazepam (Valium), with only slight structural modifications. This means that both compounds are pharmacologically identical, except that halazepam is shorter-acting and less prone to cause side effects.
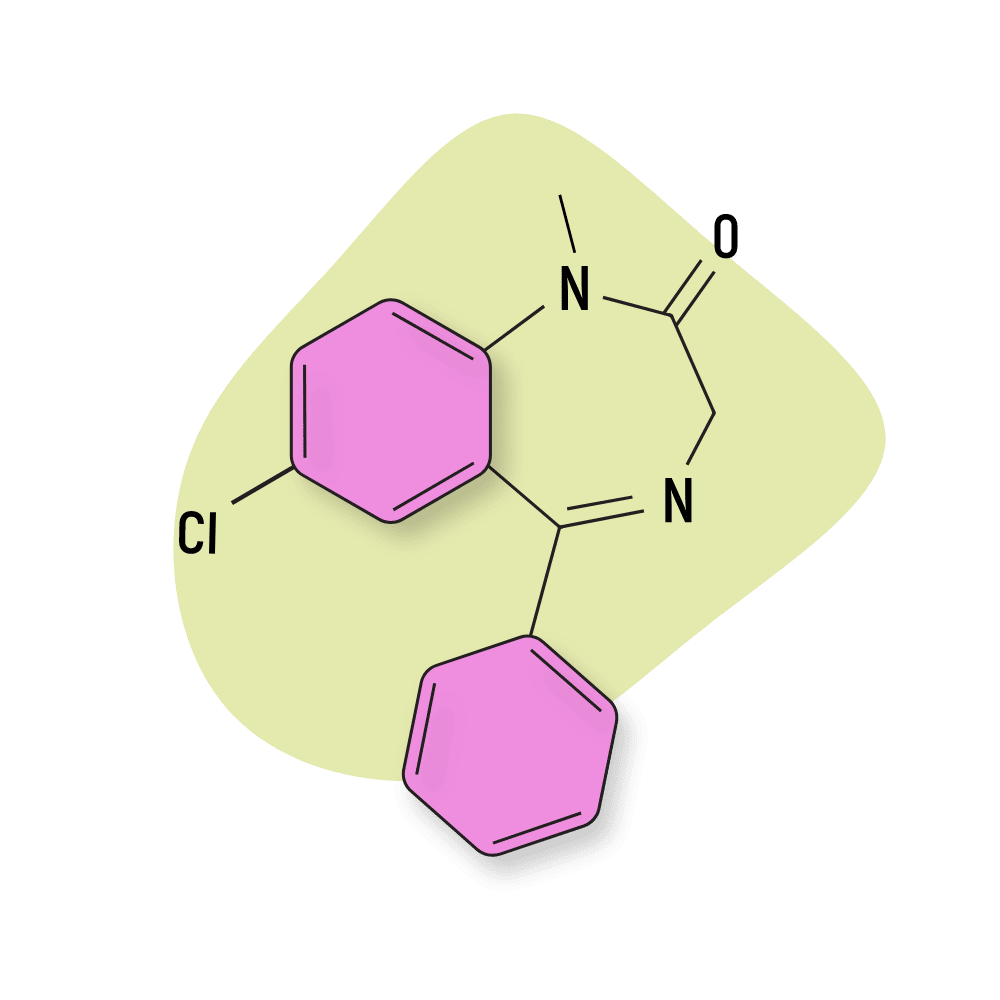
Chlordiazepoxide
Halazepam also shares this high degree of similarity with chlordiazepoxide (Librium), which was the first benzodiazepine to be synthesized and approved. The major differences are chlordiazepoxide is more potent and has a longer duration of action.
Natural Alternatives to Benzodiazepines
Want to know about some of the most popular natural alternatives to benzodiazepines?
Unfortunately, no herb or supplement will offer anywhere near the potency of a prescription benzodiazepine. However, some excellent options may work enough to avoid taking benzos in the first place or help users wean themselves off the drug slowly.
Kava
Kava (Piper methysticum) is a tropical plant species recently praised by the WHO for its natural anxiolytic and sedative benefits. Kava interacts with GABA receptors similarly to benzodiazepines to produce its effects [6] and possesses a little-seen trait where the more you use it, the more powerful its effects become. Researchers are still attempting to understand this feature.
Kratom
Another tropical plant species, kratom (Mitragyna speciosa), is a natural compound used by indigenous peoples in Southeast Asia for centuries due to its potent pharmacological capabilities. Kratom boasts a wide breadth of effects, acting as a stimulant and a euphoric in low substances. However, as more kratom is consumed, it takes on analgesic, anxiolytic, and sedative properties [7].
The problem with kratom is that, among plant-based compounds, it has more liability to induce dependence and withdrawal symptoms. This is likely because kratom interacts with the body’s opioid receptors.

Halazepam FAQs
Should halazepam be used during pregnancy?
No, halazepam is not suitable for use during pregnancy or lactation.
Does halazepam produce some of the euphoric effects of diazepam?
According to studies, halazepam does not produce these effects [8].
References
- R.S. Vardanyan, V.J. Hruby, 5 – Anxiolytics (Tranquilizers), Editor(s): R.S. Vardanyan, V.J. Hruby, Synthesis of Essential Drugs, Elsevier, 2006, Pages 69-82, ISBN 9780444521668
- John A. Davies, Halazepam, Editor(s): S.J. Enna, David B. Bylund, xPharm: The Comprehensive Pharmacology Reference, Elsevier, 2007, Pages 1-4, ISBN 9780080552323
- Willow, M., Kuenzel, E. A., & Catterall, W. A. (1984). Inhibition of voltage-sensitive sodium channels in neuroblastoma cells and synaptosomes by the anticonvulsant drugs diphenylhydantoin and carbamazepine. Molecular pharmacology, 25(2), 228-234.
- Papadopoulos, V., Baraldi, M., Guilarte, T. R., Knudsen, T. B., Lacapère, J. J., Lindemann, P., … & Gavish, M. (2006). Translocator protein (18 kDa): new nomenclature for the peripheral-type benzodiazepine receptor based on its structure and molecular function. Trends in pharmacological sciences, 27(8), 402-409.
- Fann, W. E., Pitts, W. M., & Wheless, J. C. (1982). Pharmacology, efficacy, and adverse effects of halazepam, a new benzodiazepine. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy, 2(2), 72-79.
- Pittler, M. H., & Ernst, E. (2003). Kava extract for treating anxiety. Cochrane Depression, Anxiety and Neurosis Group. Cochrane Database Syst Rev, 3.
- Eastlack, S. C., Cornett, E. M., & Kaye, A. D. (2020). Kratom—Pharmacology, clinical implications, and outlook: a comprehensive review. Pain and therapy, 9(1), 55-69.
- Ciraulo, D. A., & Oldham, M. (2014). Sedative hypnotics. In The Effects of Drug Abuse on the Human Nervous System (pp. 499-532). Academic Press.